EDITORIALS
The journey to greener vascular surgery
The Vascular and Endovascular Research Network,1 Sandford B,2,3 Garnham A3-5
The consequences of climate change pose a significant threat to health and healthcare systems globally. The increase in air pollution, temperatures and natural disasters along with the shift in patterns of infectious disease are leading to an increased disease burden.1,2 Unless urgent action is taken to mitigate climate change, the health consequences are projected to deteriorate further.3 Specific to vascular disease, the fluctuations in temperature and reduction in air quality have been associated with an increased cardiovascular morbidity and mortality.4 Thus, the continued impact of climate change, along with other disease epidemics such as diabetes, has the potential to increase the vascular disease burden. With this in mind, we need to work together as a vascular community to limit our contribution to climate change whilst continuing to manage our individual patients and vascular services.
In 2020 the NHS pledged to continue tackling healthcare-related carbon emissions and achieve carbon neutrality by 2045.5 Despite the significant progress that has been made, it is estimated that healthcare systems continue to contribute 4.9% of carbon emissions worldwide.6 A healthcare system’s carbon footprint is influenced by several components, from staff and patient travel to the resources and technologies used daily. Surgery is a major contributor to healthcare’s carbon footprint, with operating theatres being responsible for up to 25% of a hospital’s carbon output.7,8 Operating theatres are resource-intensive environments, so to an extent this is expected. However, it is estimated that, on average, the carbon emissions generated by a single case in the UK is 173 kg CO2e, which equates to driving approximately 480 miles in a petrol-fuelled car.9 If we consider the other elements of the entire patient journey from preoperative consultations and diagnostic tests to perioperative hospital stays, the carbon emissions generated from a single case are much higher.
How can we develop carbon-neutral vascular services?
Achieving more environmentally sustainable vascular practices will involve addressing several factors, as shown in Figure 1.
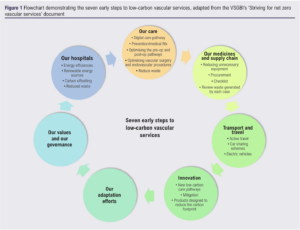
By continuing to promote vascular research and education, we can optimise public health interventions and preventative medical management strategies for patients with vascular diseases. These will reduce the burden of vascular disease and the need for extensive surgical interventions. Increased staff awareness and training in greener practices may also lead to a reduced carbon footprint, along with institutional incentives to reduce the environmental impact of hospitals.
In recent years, many vascular surgery units in the UK have developed ‘one-stop’ clinics. These clinics facilitate rapid patient consultations, assessments, treatment and improve patient outcomes.10,11 In streamlining patient pathways, these clinics also minimise patient visits to the hospital, reducing travel and carbon emissions. One-stop clinics can also improve patient satisfaction. During the COVID-19 pandemic we witnessed changes in healthcare delivery, including the introduction of remote consultations and telephone clinics.12,13 These methods proved to be a safe and effective means of consultation during lockdown and minimised patient travel to hospitals for clinic appointments.14,15 Wider adoption of remote clinic pathways, as well as ‘one-stop’ clinics, have the potential to reduce the carbon footprint of vascular services further.
The four surgical Royal Colleges have also developed an Intercollegiate Green Theatre Checklist.16 This checklist addresses changes which can be made at the pre-, intra- and postoperative stages to achieve more environmentally sustainable practice. Implementation of this checklist has the potential to serve as a reminder of the changes which can be made and contribute to an overall shift in practice.16
In 2021, surgical teams from different disciplines in the UK demonstrated that it is feasible to change surgical care pathways. Changes made included reduction in the use of single use surgical equipment, which accounts for a third of surgery-related emissions, reduction in the number of unnecessary preoperative investigations, utilisation of procedure rooms, which are less energy intensive to undertake procedures that do not require the formal operating theatre environment, changes to the types of anaesthesia used, and adoption of reusable personal protective equipment. These changes led to a reduction in 133 tons of CO2e, equivalent to 38 return flights from London to Hong Kong.17
Where do we begin to achieve environmentally friendly vascular services?
We know that there are many factors that affect the carbon footprint of vascular services, and many changes which can be undertaken to make our practice greener. The COVID-19 pandemic demonstrated the ability of vascular services to adjust practice rapidly and effectively in response to a global emergency. Now that we are faced with the challenge of delivering environmentally sustainable practice, the question is not whether we would be able to make the changes, but where the best place is to start to do so.
A recent Delphi analysis focused on reducing the environmental impact of surgery shortlisted increased recycling, reduction in anaesthetic agents and greener clinical waste processing as interventions to address.6 The next step is to begin to identify specific changes in these prioritised areas that are acceptable to clinicians and patients, feasible to deliver, safe to implement and contribute to achieving favourable patient outcomes.
The shift to more environmentally sustainable practice requires a national collaborative effort to drive transformation and help the NHS reach the ‘net zero’ target. For the vascular community to enact meaningful changes, it is paramount to first gain an understanding of current practices across vascular services, identify the potential improvements, and recognise the perceived obstacles to change.
Hence, the Vascular and Endovascular Research Network (VERN), in conjunction with the Vascular Society of Great Britain and Ireland (VSGBI) and the Royal College of Surgeons of Edinburgh Vascular Surgical Specialty Board (RCSEd Vascular SSB), are working together to identify the ways that vascular surgery can lessen our impact on the environment while maintaining excellent healthcare standards. The first task is to understand how individuals, spread across a wide geographical area with varying resources and patient populations, think vascular surgery can be feasibility changed to be more environmentally sustainable and establish a baseline understanding of practice in Trusts and Health Boards across the UK. The ‘Greener Vascular Surgery’ survey seeks to identify practical and financially viable interventions that can be implemented, whilst not compromising patient care, and seeks to uncover any potential barriers to change. We ask you all to complete this survey and join us to achieve a greener future for vascular surgery. Link to the survey: https://york.qualtrics.com/jfe/form/SV_6QIqazYZJMwwUjc
The QR code to the survey is shown in Figure 2.

*The Vascular and Endovascular Research Network: Louise Hitchman (Hull York Medical School); Brenig Gwilym (Aneurin Bevin University Health Board); Nina Al-Saadi (Black Country Vascular Network); Panagiota Birmpili (Hull York Medical School); Aminder Singh (University of Cambridge); Matthew Machin (Imperial College London); Robert Blair (Royal Victoria Hospital); Katherine Hurndall (The Royal Free Hospital); Lauren Shelmerdine (Newcastle University); Joseph Shalhoub (Imperial College London); Dave Bosanquet (Aneurin Bevin University Health Board); Nikesh Dattani (University Hospital of Leicester); Athanasios Saratzis (University of Leicester); Sara Onida (Imperial College London); Ruth Benson (University of Otago); Sandip Nandhra (Northern Vascular Centre, Freeman Hospital); Graeme Ambler (University of Bristol).
Article DOI:
Journal Reference:
J.Vasc.Soc.G.B.Irel. 2023;2(4):197-199
Publication date:
July 17, 2023
Author Affiliations:
1. Vascular and Endovascular Research Network*
2. Vascular Surgery Department, Guy’s and St Thomas’ NHS Trust, London, UK
3. Royal College of Surgeons of Edinburgh Surgical Speciality Board, Edinburgh, UK
4. General and Vascular Surgery Department, Black Country Vascular Network, West Midlands, UK
5. Vascular Society of Great Britain and Ireland, UK
Corresponding author:
Nina Al-Saadi
Vascular Surgery Department, Russells Hall Hospital,
Black Country Vascular Network, West Midlands DY1 2HQ,
UK
Email: [email protected]











