ABSTRACTS
VS ASM 2022 Prize/Highest Scoring Abstracts
The Vascular Societies’ Annual Scientific Meeting 2022, in conjunction with the VSGBI, BACPAR, SVN and SVT, took place at the Hilton Brighton Metropole, on the 23rd-25th November 2022. Here are the 2023 prize/highest scoring abstracts.
VS – Sol Cohen Prize
VO46 – The Limb-related Complications of Injecting Drug Use and the Collateral Consequences for Vascular Surgery: The East of Scotland Experience, a Nine-year Retrospective Cohort
MacLeod C1,2, O’Neill H1, Flett M1, Guthrie G1, Khan F2, Radley A2,3, Nagy J1, Suttie S1
1East of Scotland Vascular Network (ESVN), NHS Tayside, 2School of Medicine, University of Dundee , 3Directorate of Public Health, NHS Tayside
The UK has one the highest rates of illicit drug use in Europe. People who inject drugs (PWID) are at risk of a range of injecting-related infections and injuries that can threaten life and limb. This study aimed to characterise the limb-related complications of injecting drug use. Retrospective data collection between 01/12/2011-31/12/2020. Patients were identified through discharge codes and a prospective vascular operative database. Demographic and admission details were extracted from electronic records and a database created. Two diagnoses could be recorded, reflecting the realities of clinical practice. There were 805 admissions for 445 patients (1-10 admissions/ patient): mean age 37.5 (21.2-61.5) years and 488 (60.6%; 277 patients, 62.2%) were male. Admissions were generated by: 333 groin abscesses; 75 other abscesses; 109 pseudoaneurysms; 126 necrotising soft tissue infections; 137 cellulitis cases; 168 deep venous thromboses (DVT); 59 infected DVTs and 138 other pathologies. Surgical specialties managed 570 (70.8%) admissions, with vascular surgery managing 412 (51.2%; 72.3% of all surgical admissions). Surgery was required for 409 admissions (50.8%), with 534 operations performed (1-7/ admission). There were 31 lower limb amputations. During follow-up 97 (21.8%) patients died, mean age 43.6 (26.8-62.8). Limb-related complications of injecting drug use represent a substantial burden for vascular surgery.
VS – BJS Prize
VO59 – Repair for Infrarenal Aortic Abdominal Aortic Aneurysms, a Nationwide Study
Pouncey A1, Nicola M1, Martin G1, Bicknell C1, Powell J1
1Imperial College London
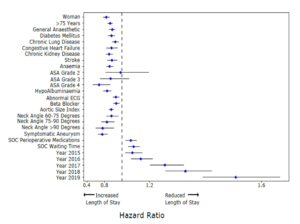
Introduction Length of hospital stay (LOS) for endovascular infra-renal abdominal aortic aneurysm repair (EVAR), is a major driver of cost and reported to be longer for women. This study investigates drivers of LOS and why women stay longer for EVAR. Methods Examination of National Vascular Registry elective EVAR patients, 2014-2020. Survival analysis conducted, censoring for in-hospital death. Cox proportional hazard modelling utilised to assess sex-specific difference in LOS adjusting for age, co-morbidity, anaesthetic, year and standard-of-care. Results 14,050 (12,518 men:1532 women) patients received elective EVAR. LOS was longer for women (restricted-mean 6.55 (standard error (SE)0.59) vs. 4.49 (SE0.12) days, p<0.001). Following multivariable adjustment, early hospital discharge remained less likely for women (Hazard Ratio (HR) 0.81, 95%CI:0.78-0.87). General anaesthetic (HR 0.89 (95%CI:0.86-0.93), age >75 years (HR 0.80, 95%CI 0.84-0.90), co-morbidity and anatomical complexity were associated with increased LOS. Treatment within waiting-times and receipt of peri-operative antibiotics/ thromboprophylaxis were associated with reduced LOS. Between 2014-2019 LOS reduced for both sexes (restricted-mean change -2.46 vs. -2.18 days; HR 1.54, 95%CI 1.44-1.64). Conclusion Women have increased LOS for EVAR, despite adjustment for co-morbidity, standard-of-care and advanced clinical practice. Identification of additional drivers of LOS for women is needed to facilitate fast-track pathways and improve quality-of-care.
VS – Poster Prize
P36 – Optimising secondary prevention in patients undergoing carotid intervention (CI) – A Single Centre Cohort Study
Kwan J1, Sood M1, Stocco F1, Bailey M1, Coughlin P1, Scott J1
1Leeds Vascular Institute
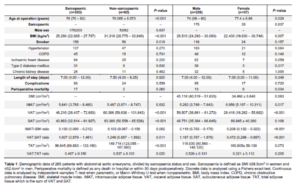
Background Stroke/TIA patients should receive best medical therapy (BMT; antithrombotic therapy (ATT) and lipid lowering therapy (LLT)). This includes high-intensity statins (HIS), aiming for LDL-C <1.8mmol/L. We explored BMT in patients undergoing CI on admission prior to intervention, at discharge, and 1 year post intervention. Method 205 patients underwent CI (01/01/18–31/12/20). Differences between time points were assessed with McNemar test. Results There were 137 men (67%), median age 73 (CI: carotid endarterectomy n=175; carotid stent n=30). Increases in prescription of ATT (50%vs96%, p<0.001), statins (65%vs93%, p<0.001) and HIS (47%vs83%, p<0.001) were observed at discharge compared to pre-intervention but no differences were seen at 1 year. At 1 year, 8 patients were not taking statin therapy, 6 were allergic and 3 prescribed Ezetimibe. At 1 year, there was significant improvement in median LDL-C (2.4mmol/L, IQR(1.9-3.3)vs.1.6mmol/L, (1.2-2.0), and proportion of patients achieving an LDL-C of <1.8mmol/L (21%vs59%,p=0.003) compared to pre-admission. In patients with LDL-C>1.8mmol/L, 92% had scope for LLT up-titration. Conclusion Patients undergoing carotid intervention receive appropriate BMT whilst in-patient. This led to improved lipid control in a substantial proportion. A minority fail to achieve recommended LDL-C targets. Reasons for this need to be understood to allow for optimal risk reduction.
VS – The Richard Wood Memorial Prize
VO82 – A single-centre retrospective hypothesis-generating study investigating Computed Tomography-based body composition metrics in a cohort of aortic aneurysm patients
Koh A1, Yang Q1, Boshier P2, Hanna L2,3, Gibbs R2,3
1School of Medicine, Imperial College London, 2Department of Surgery and Cancer, Imperial College London, 3Imperial Vascular Unit, Imperial College Healthcare NHS Trust
Introduction aortic aneurysms (AAA) remains unknown. This study explored the patterns of Computed Tomography-based body composition (CTBC) metrics in AAA patients, and their associations with outcomes. Methods We included 265 patients who received open or endovascular AAA repair from 2015 to 2020 at a single institution. Cross-sectional surface areas of skeletal muscle (SMI), intramuscular (IMAT), visceral (VAT), and subcutaneous (SAT) adipose tissues at the L3 vertebral level were obtained from preoperative CT scans. Sarcopaenia was defined as SMI <38.5cm2 in women and <52.4cm2 in men. Outcomes included hospital length of stay, postoperative complications, and peri-operative mortality (in hospital or within 30 days). Results Sarcopaenic patients had less total adipose tissue (p<0.001), lower VAT/SAT ratios (p=0.011), and higher IMAT/SMI ratios (p=0.002). Lower SMI was associated with peri-operative mortality (p=0.011). Peri-operative mortality was higher among female patients (p=0.027), who had higher IMAT (p=0.017) and IMAT/SMI ratios (p<0.001), and lower VAT/SAT ratios (p<0.001) compared to male patients. Conclusions Sarcopaenia is often accompanied by high IMAT and low VAT and is associated with peri-operative mortality. CTBC differences between men and women may contribute to different mortality rates.
VS – Venous Prize
VO93 – Impact of the NHS Evidence Based Intervention Programme on access to NICE recommended Varicose Vein Treatment
Hitchman L1, Mohamed A1, Smith G1, Pymer S1, Chetter I1, Forsyth J2, Carradice D1
1Hull York Medical School, 2Leeds University Teaching Hospital NHS Trust
Background A previous study demonstrated widespread non-compliance of Clinical Commissioning Group (CCG) policies with NICE guidelines leading to geographic variation in access to varicose vein treatment. The Evidence Based Intervention (EBI) programme aimed to improve care quality. This study assesses the impact of EBI. Method CCG policies were obtained before and after EBI and categorised by two independent reviewers into levels of compliance with NICE CG168 (green/amber/red). Hospital episode statistics were compared with the NICE commissioning model predictions. Results The number of green policies fell from 33.5%(64) to 28.8%(55) in 2019, amber policies increased from 55.5%(106) to 62.3%(119) and red policies remained static (8.9% (17) vs. 8.4%(16)). Over this period 7.3%(14) changed their policy to become fully compliant, but 33.0%(63) changed their policy to become less compliant. Common deviations were to restrict based on clinical severity 51.8%(99) or delay for conservative management 22.5%(43). Nationally the proportion of interventions performed fell from 43.6% to 37.5% of predicted levels, with an estimated loss in net health benefit of £174.6million. Conclusion The EBI programme is not associated with improvement in commissioning policy or unwarranted variation, with most patients remaining unable to access NICE recommended treatment in England prior to the SARS Cov-2 pandemic.
SVN – James Purdie Prize
NO4 – Use of Biodegradable Temporising Matrix (BTM) in vascular surgery
Harris L1, Thapar A1, Graham A1, Emmanuel A1, Mallick A1
1Mid And South Essex NHS Trust
Introduction
Open wounds over vascular grafts and bone commonly result in graft infection, osteomyelitis and subsequent amputation (1)(2). Traditionally these wounds would be left to heal by secondary intention +/- antibiotics, leading to prolonged treatment. NovoSorb Biogradable Temporising Matrix (BTM) by PolyNovo is a synthetic polymer that can temporarily close the wound allowing for new tissue generation (3). We used BTM in 5 vascular patients for which conventional wound cover was not an option, a first in the UK.
Method
1. Exposed prosthetic graft
2. Exposed vein graft anastomosis
3. Open below knee amputation with bone exposure
4. Open transmetatarsal amputation with bone exposure
5. Post calcanectomy for osteomyelitis with exposed calcaneum
Results
Wounds ranged from surgical bypass wounds to amputation sites. In four cases the BTM integrated well into the wound bed by 6 weeks, covering the critical structures. In the one treatment failure the wound closed by secondary intention.
Conclusion
BTM provides a low-cost option for covering high risk structures, where flaps or grafts are not possible. The thickness of coverage is limited. Further analysis of application technique and patient selection criteria needs to be carried out as well as longer term outcomes.
SVT – Best Scientific Presentation
TO24 – A reflection of measuring and applying qualitative approaches to a Vascular Ultrasound
Lab Zakikhani N1
1St Georges University Hospital
Throughout my experiences of working within healthcare, the processes and attention of measuring qualitative data in a clinical setting has taken a back seat when compared to the huge emphasis on quantitative approaches. For example, focus tends to favour on how many scans can be performed on an ultrasound machine per day rather than also assessing patient satisfaction and re-designing patient pathways to facilitate patient centred care. Vascular sonographers are a vital cog in the patient pathway in assisting in the diagnosis of diseases. However should they wish, they can also play a major role in helping facilitate the qualitative measures to improve patient care given their involvement in large webs of care and their patient facing roles. This talk is a reflection of my application of qualitative aspects of healthcare through my learning on the Elizabeth Garrett Anderson Program (MSc Healthcare leadership). Topics of reflection include my experiences in the power of honest conversations, the importance of story telling to extract information, sub-conscious behaviours, perceptions, looking beyond the tip of the iceberg the and tools to help facilitate qualitative sciences in a Vascular Ultrasound Lab.
SVT – Best recently completed research presentation
TO13 – Transthoracic ultrasound evaluation of thoracic aortic aneurysms
Davey H1,2, Enemosah I1, Rogan C1, Patel P1, Patterson B1
1University Hospital Southampton, 2Newcastle University
Background Thoracic aortic aneurysms (TAA) can be asymptomatic and life- threatening if they rupture. They are currently detected using computed tomography (CT) which is expensive and uses radiation. A previous study found that ultrasound has the potential to be used as a diagnostic modality for TAA. However, further validation of this methodology is required. Methods 15 patients (9 with TAA and 6 controls) had a single ultrasound assessment of the thoracic aorta performed by a single vascular scientist. The maximum diameter at the ascending aorta, aortic arch, mid and distal descending thoracic aorta was measured and compared to diameters from a CT scan at thresholds of 35mm and 40mm. Results The thoracic aorta was visualised in all 15 patients. At 35mm, the sensitivity and specificity were 100% and 85% and at 40mm it was 78% and 100%. The Bland-Altman plot showed good agreement between ultrasound and CT measurements for the maximum diameter and at the aortic arch, mid and distal descending thoracic aorta. Conclusion There is good visualisation of the thoracic aorta using ultrasound with high sensitivity and specificity at both 35mm and 40mm. Results of this study suggest that ultrasound has a potential to be used to assess TAA.
SVT – Best research proposal
TO3 – An audit to determine whether patients receive two forms of carotid imaging pre-operatively when carotid endarterectomy (CEA) is being considered, in line with the European Society for Vascular Surgery (ESVS) 2017 Clinical Practice Guidelines.
Alderson E1
1Cambridge University Hospitals NHS Foundation Trust
Introduction The 2017 ESVS Clinical Practice guidelines state two forms of imaging are recommended pre-CEA; this can be a combination of duplex ultrasound (DUS), computed tomographic angiography and magnetic resonance angiography, or two DUS performed by different operators. Methods Data was collected retrospectively from the National Vascular Registry to identify patients who underwent CEA between January 2019-December 2021 (n=205). No exclusion criteria were applied. EPIC electronic patient record system was used to obtain relevant data from patients’ files including: pre-CEA imaging modalities, complications, outcomes and patient demographics. Data will be analysed using descriptive statistics and chi squared and Mann-Whitney statistical tests. Results Between January 2019-December 2021, 87.3% of patients met the ESVS guidelines. Of the 12.6% who did not comply with the guidelines; 80.8% received one form of imaging and 19.2% received two DUS performed by the same operator. Conclusion No single reason was identified to explain non-compliance with the 2017 ESVS guideline. Results were disseminated to all interested stakeholders and a common point for intervention in the patient pathway was identified. A six month time lapse (June-December 2022) before re-auditing will enable assessment of the effectiveness of interventions to improve guideline compliance.
BACPAR – Highest scoring abstract submission
BO3 – Sharing stories of lower limb amputation in practice: An exploration into the relatability, usability, and implementation of an animation video package across UK rehabilitation services
Taylor E1, Leggat F2
1St Mary’s University, 2St George’s, University of London
In 2015, a collaboration between academia and an NHS limb loss rehabilitation centre began. Presented through BACPAR conferences and journal pieces, the partnership has produced research which includes the construction of five narrative trajectories within major lower limb amputation (MLLA) and the translation of these narratives into animation videos. Findings indicated that exposure to the narrative raised less experienced therapists’ awareness of MLLA journeys and increase their preparedness for patient care. When presented in a group activity, people with MLLA connected and resonated with the videos, developed knowledge about what to expect following rehabilitation, and identify helpful behaviours to action. However, it is not known how these videos relate or may be useful to those in differing rehabilitation environments across the UK. The aim of the presentation is not only to describe, but to do the animation video activity with BACPAR delegates. This will enable delegates to experience the videos as people in MLLA rehabilitation would do. Delegates will be encouraged to discuss and reflect upon the experience with colleagues in the world café event. It is hoped the activity will prompt conversation into the relatability, usability, and implementation of the videos across regional amputee rehabilitation service.
Article DOI:
Journal Reference:
J.Vasc.Soc.G.B.Irel. 2023;2(2):121-125
Publication date:
February 28, 2023











