WINNING ESSAYS
Rouleaux Club Winning Essay 2024
The Rouleaux Club run an annual essay competition to help promote interest in vascular surgery. Entrants are asked to write 1,500 words on one of three topics selected by the RC Executive. The essays are marked by the committee and the prizes are awarded to the best essay at the annual Vascular Society meeting. There are two prize categories, one for medical students and another for junior doctors. Following the Vascular Societies GB&I Annual Scientific Meeting, the winning essays will be published in the journal.
STUDENT CATEGORY
Should vascular surgery trainees be allowed to sub-specialise during training?
Oladimeji John Abiodun, University of Nottingham, 5th Year medical student
Introduction
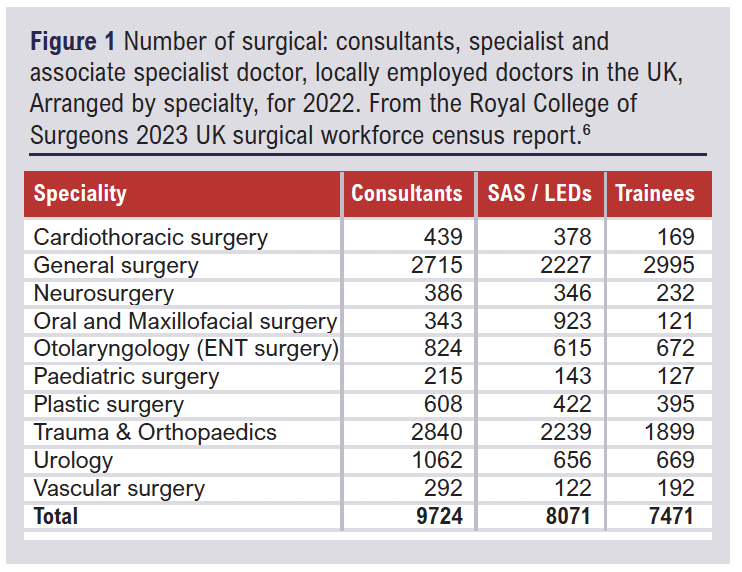
“The Vascular Surgeon” as a distinct entity, is a novel concept in the UK, only formalising in 2013, with the introduction of the specialty vascular training programme.1 Following the conventional pathway, it takes a trainee a minimum of 8 years post foundation training to achieve the competencies required to become a vascular consultant.2,3 Initially encompassed within general surgery, the increased demand and expertise needed for vascular intervention brought about a need for separation.1 A 20-year predictive study foresaw an increase in vascular procedures of 40.5% over a 20-year period, (2000-2020), with a 5.5.% increase in patients over 65, a group at high risk of vascular disease.4,5 Between the years 2000-2020 the number of patients requiring vascular surgical intervention were all predicted to show a percentage increase: claudication 35.4%, critical limb ischaemia 44.2%, carotid surgery 34.0%, abdominal aortic aneurysm 40.7%, acute limb ischaemia 45.0% and access surgery 27.4%.4 Despite the projected increase in vascular procedures,4 vascular surgery makes up one of the smaller surgical cohorts.6 Data published by the Royal College of Surgeons showed that in 2022 there were 9,724 consultant surgeons in the UK (Figure 1).6 Out of this population, there were only 292 vascular consultants and 192 trainees.6 As with most specialties within the NHS, there is an evident need for more vascular trainees.7
The ever-expanding nature of surgery meant that the dawn of independent vascular consultants was inevitably followed by the need for sub-specialisation within vascular surgery. The current system takes a vascular trainee through each aspect of vascular and endovascular surgery.3,8 Upon completion, a consultant is able to home in on a specific domain within the field should they choose to do so. This includes, but is not limited to trauma surgery, endovascular aortic surgery, access surgery, venous and endo-venous training, thoracic outlet specialist & sarcoma specialist.9,10 The drive towards sub-specialisation is not unique to the UK, for example 70% of General surgery residents in the United States pursue further specialist training after completion of their general surgery programmes.11,12 This begs the question, is there a need to delay the commencement of a trainees sub-specialist training & how could early sub-specialisation impact outcomes for patients and doctors?
Benefit to the doctor
Examination of the literature shows that early specialisation can lead to perceived improvement in lifestyle, job security, added independence and financial recompense.11,13,14 Furthermore, there is a growing appetite for surgical trainees to achieve stability earlier in their careers, an eagerness amongst some trainees for the length of training to decrease, and a desire to sub-specialise during training.6,15,16 Early specialisation could help combat the growing levels of burnout recorded amongst trainees.15,16 Whilst fears that early differentiation of trainees can lead to an asymmetrical skillset for the future consultants, this may not be entirely the case. A 2002 – 2017 analysis of case logs for 231 orthopaedic trainees found that residents who chose spine surgery (108.4±50.7 vs 74.4±60.2, p<.01), hand surgery (242.2±92.9 vs 194.3±78.2, p<.01), and sports medicine (278.5±105.8 vs 229.0±93.9, p<.01) performed more procedures in their chosen fields than their colleagues. However, for total joint arthroplasty (p=.18) and foot and ankle surgery (p=.46), there was no significant difference in the number of cases between residents who chose the sub-specialty and those who did not.17 Whilst this study is limited in its range of specialities analysed, it does indicate that if properly structured, trainees are able to sub-specialise and still retain an appropriate breadth of surgical exposure.
Benefit to the patient
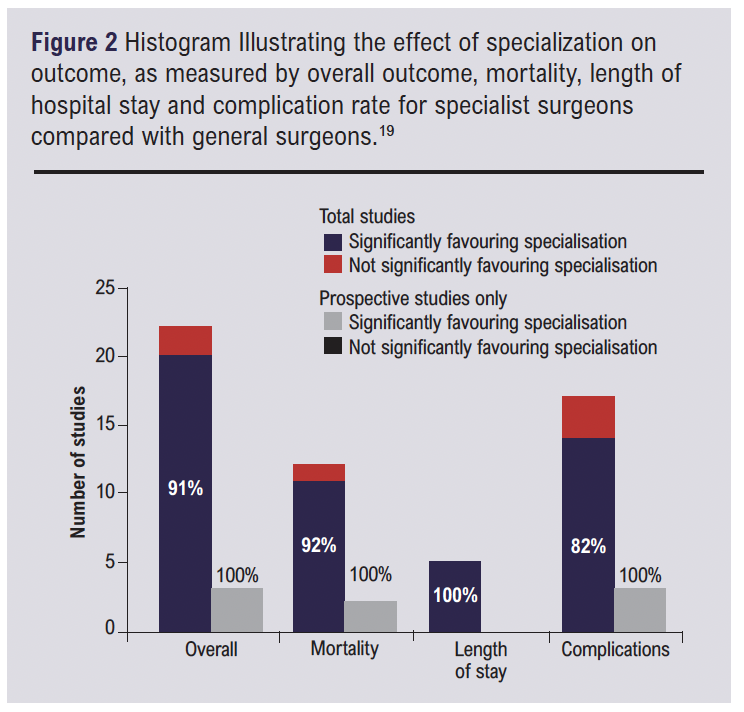
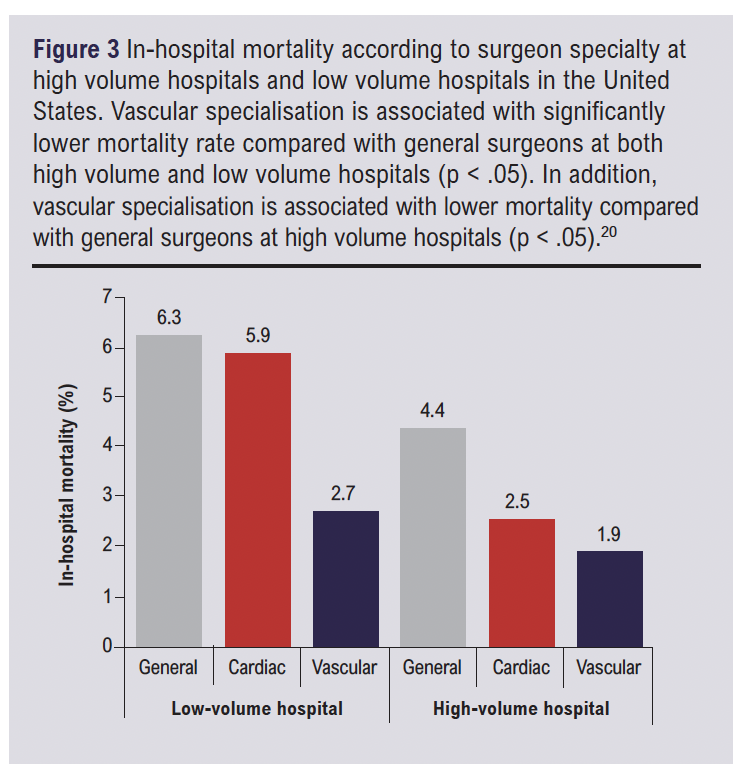
A small study on the effect of a surgeon’s seniority and subspeciality interest on mortality, found that surgery carried out by a surgeon without subspeciality interest related to the pathology was associated with a higher risk of postoperative mortality compared with a surgeon with subspeciality interest (OR: 1.38, p < 0.00001).18 A systematic literature review of 22 studies and 144,241 patients found in 91% of cases, specialist surgeons had significantly better outcomes when compared to general surgeons performing the same procedure.19 This was quantified with a lower mortality rate in 11 of 12 studies (92%), shorter hospital stay in five of five studies and fewer complication rates in 14 of 17 studies (82 %) (Figure 2). This favours the notion that allowing trainees to subspecialise earlier, would increase the pool of effective clinicians best suited to treat specific caseloads. Furthermore, a study into procedural specialisation showed mortality following abdominal aortic aneurysm repairs were lowest when carried out by vascular specialists (2.2%) compared to cardiac (4.0%) and general surgeons (5.5%, p<0.001) (Figure 3).20 This principle could then be extrapolated further for sub-specialisation within vascular surgery, where a trainee specialising in major trauma will be better suited to deal with, for example, a road-traffic accident, opposed to one focused primarily on endovascular techniques. It appears logical to infer from some literature that earlier sub specialisation could contribute to better patient outcomes.
Negatives to the doctor
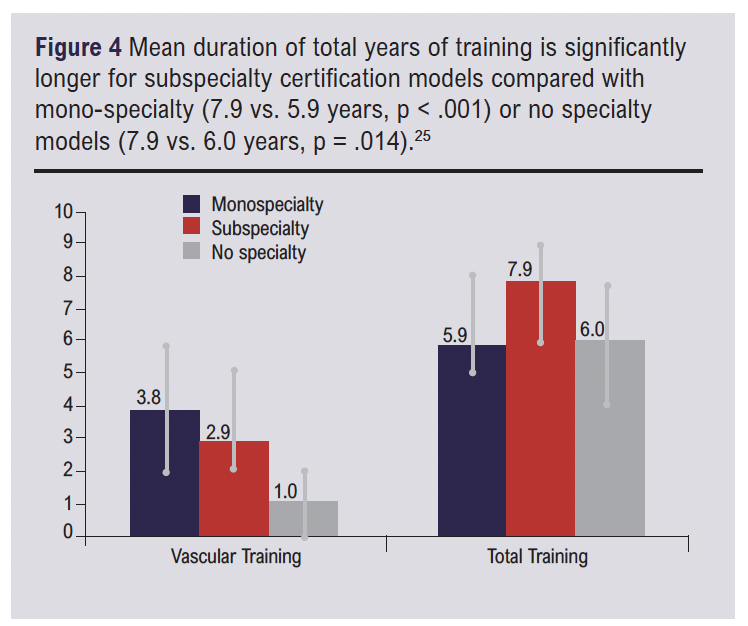
It is well established that theatre time amongst trainees has diminished significantly since the start of the 21st century, as much as 50% in some cases, and there is significant variation in the opportunity for trainees to carry out basic procedures.21-23 While new methods such as simulation – based medical training have shown to help prevent the decay of surgical skills,21,24 a systematic literature review by Higgins et al showed there are currently no substitutes comparable to “time in theatre developing surgical skills”.21 The UK has one of the longest training times for vascular surgeons across Europe,25 and in instances where vascular surgery is a subspecialty, average training times are almost 2 years longer.25 Studies also show that countries who view vascular surgery as a sub-specialty, have longer over all training times compared to those who don’t (Figure 4).25 It could be argued that further sub-specialisation would increase the years needed to achieve the necessary core surgical and specialist skills. Increased training time may deter trainees, as years taken to complete training is a key component of dissatisfaction in current doctors within surgery and medicine.6,15 Continuous sub-specialisation also narrows the working range for doctors, and may lead to them becoming less confident with their basic competencies in areas outside of their established scope of practise.26 This was one of the factors contributing to vascular surgery becoming distinct from general breast and gastrointestinal surgeons.1,27
Negatives to the patient
Over specialisation can lead to de skilling of a surgeons general skills, which may be most acutely felt when providing care for patients in the emergency setting.28 A recent evaluation of 1554 emergency cases, found 30% of 357 patients requiring complex operations, had their care overseen by a consultant whose sub-speciality did not closely match their case.28 It should be noted 72% of these cases happened out of hours and only 18% had the consultant scrubbed and in theatre. However, there are already shortages in surgeon numbers,29-31 and the added complexity of matching suitable specialist trainees and consultants to ambiguous emergency and general cases, could mean more instances of sub-optimal patient care. Looking across medicine we see several articles warning about the devolution of the generalist and enabling early entry into specialist pathways before adequate exposure to a breath of disciplines, can risk inappropriate patient diagnosis and referrals.32-34 Whilst the association may seem clear, there are limited large scale randomised controlled studies affirming that an increased level of sub specialisation results in improved clinical outcomes.
Conclusion
More research is needed to make conclusive statements about the benefit of early subspecialisation on patient care within vascular surgery. Having explored the potential positives and pitfalls, I believe trainees should be given the option to sub-specialise from the start of training, but not the requirement to. This provides flexibility for trainees who will inevitably differ based on personal circumstance. Most importantly, as with all medicine, the patient should be at the forefront of all decisions made.
References
1. Lamont P, Wyatt MG, Naylor AR. Vascular surgery: a new surgical specialty in the UK. The Bulletin of the Royal College of Surgeons of England
2015;94(7):232–33. https://doi.org/10.1308/147363512X133113141968
2. Payne T, Toms JD, Zaidi A, Thrumurthy SG. The history of surgery and surgical training in the UK. Pak J Med Sci 2021;37(5):1532-35.
https://doi.org/10.12669/pjms.37.5.4628
3. Vascular Surgery Curriculum. ISCP [Internet]. [cited 2024 Sep 28].
Available from: https://www.iscp.ac.uk/iscp/curriculum/vascular-surgery-curriculum/2-purpose/
4. Heikkinen M, Salenius JP, Auvinen O. Projected workload for a vascular service in 2020. Eur J Vasc Endovasc Surg 2000;19:351–5.
https://doi.org/10.1053/ejvs.2000.1074
5. Conrad N, Molenberghs G, Verbeke G, et al. Trends in cardiovascular disease incidence among 22 million people in the UK over 20 years: population based study. BMJ 2024;385. https://doi.org/10.1136/bmj-2023-078523
6. UK Surgical Workforce Census Report 2023 — Royal College of Surgeons [Internet]. [cited 2024 Sep 28]. Available from: https://www.rcseng.ac.uk/standards-and-research/surgical-workforce-census/
7. Harkin DW, Beard JD, Shearman CP, Wyatt MG. Predicted shortage of vascular surgeons in the United Kingdom: A matter for debate? Surgeon 2016;14(5):245–51. https://doi.org/10.1016/j.surge.2015.10.004
8. Vascular surgery curriculum – GMC [Internet]. [cited 2024 Sep 28]. Available from: https://www.gmc-uk.org/education/standards-guidance-and-curricula/curricula/vascular-surgery-curriculum
9. Vascular Surgery – Working across Wessex [Internet]. [cited 2024 Sep 25]. Available from: https://wessex.hee.nhs.uk/school-of-surgery/vascular-surgery/
10. Poultsides GA, Tran TB, Zambrano E, et al. Sarcoma resection with and without vascular reconstruction: a matched case-control study. Ann Surg 2015;262(4):632. https://doi.org/10.1097/SLA.0000000000001455
11. Schmidli J, Dick F. Specialisation within vascular surgery. Eur J Vasc Endovasc Surg 2010;39(SUPPL. 1):S15–21. https://doi.org/10.1016/j.ejvs.2009.12.013
12. Stitzenberg KB, Sheldon GF. Progressive specialization within general surgery: adding to the complexity of workforce planning. J Am Coll Surg. 2005;201(6):925–32. https://doi.org/10.1016/j.jamcollsurg.2005.06.253
13. Bell RH. Graduate education in general surgery and its related specialties and subspecialties in the United States. World J Surg 2008;32(10):2178–84. https://doi.org/10.1007/s00268-008-9658-x
14. Longo WE, Sumpio B, Duffy A, Seashore J, Udelsman R. Early specialization in surgery: the new frontier. Yale J Biol Med 2008;81:187–91.
PMID: 19099049; PMCID: PMC2605312.
15. Robinson DBT, Luton O, Mellor K, et al. Trainee perspective of the causes of stress and burnout in surgical training: a qualitative study from Wales. BMJ Open 2021;11(8):e045150. https://doi.org/10.1136/bmjopen-2020-045150
16. Johnson J, Al-Ghunaim TA, Biyani CS, Montgomery A, Morley R, O’Connor DB. Burnout in surgical trainees: a narrative review of trends, contributors, consequences and possible interventions. Indian J Surg 2022;84(Suppl 1):35.
https://doi.org/10.1007/s12262-021-03047-y
17. Mason DePasse J, Nzeogu MI, Travers C, et al. Early subspecialization in orthopedic surgery training. Orthopedics 2019;42(1):e39–43. https://doi.org/10.3928/01477447-20181109-01
18. Al-Sarireh H, Al-Sarireh A, Mann K, Hajibandeh S, Hajibandeh S. Effect of surgeon’s seniority and subspeciality interest on mortality after emergency laparotomy: A systematic review and meta-analysis. Colorectal Disease 2024;26(8):1495–504. https://doi.org/10.1111/codi.17079
19. Chowdhury MM, Dagash H, Pierro A. A systematic review of the impact of volume of surgery and specialization on patient outcome. Br J Surg 2007; 94(2):145-61. https://doi.org/10.1002/bjs.5714.
20. Dimick JB, Cowan JA, Stanley JC, Henke PK, Pronovost PJ, Upchurch GR. Surgeon specialty and provider volumes are related to outcome of intact abdominal aortic aneurysm repair in the United States. J Vasc Surg 2003; 38(4):739–44. https://doi.org/10.1016/S0741-5214(03)00470-1
21. Higgins M, Madan C, Patel R. Development and decay of procedural skills in surgery: A systematic review of the effectiveness of simulation-based medical education interventions. The Surgeon 2021;19(4):e67–77.
https://doi.org/10.1016/j.surge.2020.07.013
22. Greensmith M, Cho J, Hargest R. Changes in surgical training opportunities in Britain and South Africa. Int J Surg 2016;25:76–81.
https://doi.org/10.1016/j.ijsu.2015.11.052
23. Dunn JC, Belmont PJ, Lanzi J, et al. Arthroscopic shoulder surgical simulation training curriculum: transfer reliability and maintenance of skill over time.
J Surg Educ 2015;72(6):1118–23. https://doi.org/10.1016/j.jsurg.2015.06.021
24. Agha RA, Fowler AJ. The role and validity of surgical simulation. Int Surg 2015;100(2):350–7. https://dx.doi.org/10.9738/INTSURG-D-14-00004.1
25. Avgerinos ED. Vascular training profiles across Europe. Eur J Vasc Endovasc Surg 2013;46(6):719–25. https://doi.org/10.1016/j.ejvs.2013.08.003
26. Bass BL. Early specialization in surgical training: an old concept whose time has come? Semin Vasc Surg 2006;19(4):214–17.
https://doi.org/10.1053/j.semvascsurg.2006.08.013
27. Lamont PM, Scott DJA. The impact of shortened training times on the discipline of vascular surgery in the United Kingdom. Am J Surg 2005;190(2): 269–72. https://doi.org/10.1016/j.amjsurg.2005.05.025
28. Garner JP, Prytherch D, Senapati A, O’Leary D, Thompson MR. Sub- specialization in general surgery: the problem of providing a safe emergency general surgical service. Colorectal Disease 2006;8(4):273–7. https://doi.org/10.1111/j.1463-1318.2005.00932.x
29. More than half of UK surgical workforce says access to operating theatres is a major challenge. Royal College of Surgeons [Internet]. [cited 2024 Sep 30]. Available from: https://www.rcseng.ac.uk/news-and-events/media-centre/press-releases/surgical-workforce-census-2023/
30. Milner A, Nielsen R, Norris E. Brexit and European doctors’ decisions to leave the United Kingdom: a qualitative analysis of free-text questionnaire comments. BMC Health Serv Res 2021;21(1).
https://doi.org/10.1186/s12913-021-06201-0
31. Brexit has worsened shortage of NHS doctors, analysis shows. The Guardian [cited 2024 Sep 30]. Available from: https://www.theguardian.com/society/ 2022/nov/27/brexit-worsened-shortage-nhs-doctors-eu
32. Lumley JS. Subspecialisation in medicine. Ann Acad Med Singap 1993; 22(6):927-33. Available from: https://pubmed.ncbi.nlm.nih.gov/8129359/
33. Rouhani MJ. In the face of increasing subspecialisation, how does the specialty ensure that the management of ENT emergencies is timely, appropriate and safe? J Laryngol Otol 2016;130(6):516–20.
https://doi.org/10.1017/S0022215116007957
34. Michael CA. Subspecialisation in obstetrics and gynaecology–whither (or wither) the generalist. Ann Acad Med Singap 1990;19(6):872-4.
Available from: https://pubmed.ncbi.nlm.nih.gov/2130757/
Article DOI:
Journal Reference:
J.Vasc.Soc.G.B.Irel. 2025;4(4):238-241
Publication date:
August 28, 2025











