CASE REPORT
The first confirmed isolation of Dermabacter vaginalis from a mycotic abdominal aortic aneurysm
Williams SN,1 Wangrangsimakul T,2 Howard DPJ3,4
Abstract
Dermabacter vaginalis is a recently identified extremely rare bacterial species not previously implicated as an agent in any disease process. This report covers the first recorded case of D. vaginalis isolated from periaortic fluid during surgical repair of a mycotic abdominal aortic aneurysm. The patient was successfully treated with a surgical approach combined with an antibiotic regimen tailored to the sensitivities of D. vaginalis.
Introduction
Bacteria of the genus Dermabacter are considered skin colonisers. Dermabacter hominis, the first species characterised, has been isolated from a variety of clinical specimens including blood, suggesting its potential as an opportunistic pathogen.1 Dermabacter vaginalis was first isolated in 2016 from the vaginal fluid of a woman in Korea.2 Subsequently, the genome of D. vaginalis has been sequenced,3 along with the identification of unique metabolites that it produces.4 Following its initial discovery, this strain has not been isolated from another human source, and thus no role in pathogenicity has been described to date for D. vaginalis. We report the isolation of D. vaginalis following surgical repair of a mycotic aortic aneurysm.
Case presentation
A 74-year-old man presented to the emergency department in January 2025 with a two-day history of severe abdominal pain which had worsened overnight and had radiated to the back. He had also vomited once but displayed no other symptoms. These features were deemed suggestive of a mycotic abdominal aortic aneurysm. He had recovered from a cold 10 days earlier and had several vascular risk factors including hypertension, diabetes mellitus, previous stroke and myocardial infarction. His white cell count was 14×109/L and a CT scan confirmed the presence of a 3.7 cm diameter infrarenal aneurysm with evidence of aortitis. An initial strategy of IV antibiotic therapy without surgical intervention was commenced. However, the following morning the patient complained of worsening abdominal pain with ongoing fever overnight. Repeat CT angiography revealed rapid expansion of the aortic aneurysm to 4.2 cm with worsening fat stranding confirmed (Figure 1). The patient was therefore counselled for emergency open aneurysm repair.

A standard midline laparotomy incision was made and the retroperitoneum opened. Collateral and lumbar vessels were ligated and the renal and common iliac arteries were isolated. The aorta was clamped above the left and below the right renal artery. Extensive inflammation of the aortic aneurysm and the surrounding tissues was visible (Figure 2). The repair was completed using a silver impregnated Dacron tube graft and took a total of 4 hours and 50 minutes.

Postoperatively the patient recovered well with minimal complications. Periaortic fluid samples cultured D. vaginalis, which was reported as susceptible to higher doses of penicillin, tetracycline, linezolid, rifampicin, vancomycin and resistant to ciprofloxacin. Blood cultures were negative after five days. He was treated with six weeks of IV ceftriaxone 2 g once daily via a peripherally inserted central catheter followed by long-term oral doxycycline 100 mg twice daily, as guided by input from infectious diseases. The patient was discharged nine days postoperatively with safety-netting advice in place and follow-up arranged with both vascular and infectious diseases specialists.
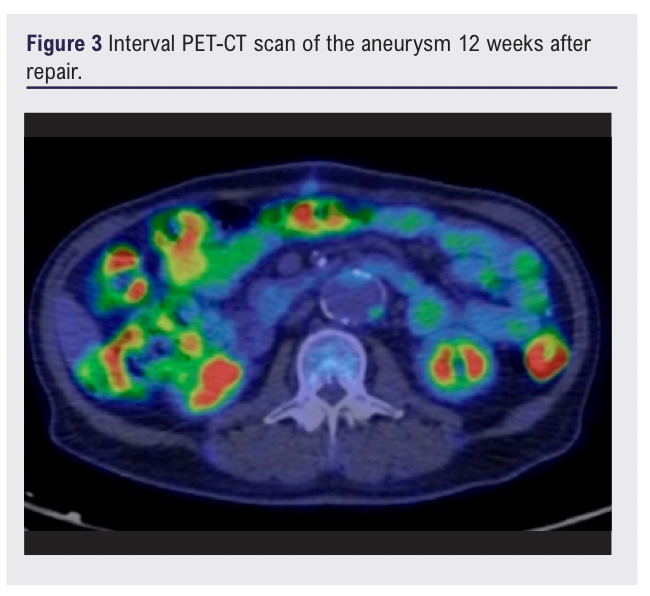
An interval PET-CT scan (Figure 3) was performed around 12 weeks after surgical repair which showed patchy uptake within the aortic graft, likely to represent postoperative changes post-intervention. Clinic review five months after surgery was reassuring with the patient recovering well and tolerating oral doxycycline along with normal blood tests. The agreed plan was for a further interval PET-CT scan at 10 months after surgery (November 2025) with subsequent review and discussion in clinic regarding whether to continue or stop antibiotic suppression at that point.
Discussion
Mycotic aneurysms are rare, causing as few as 0.6–2% of abdominal aortic aneurysms, with evidence consistently showing Staphylococcus aureus to be the most commonly involved pathogen in high-income settings.5,6 Several other bacterial species – and more rarely some fungal agents – have been shown to cause mycotic aortic aneurysms, but D. vaginalis represents a potential novel player in aneurysm pathology. Given the relatively recent discovery of D. vaginalis and the low global incidence of mycotic aneurysms, it is unsurprising that no such cases have been described previously. Data from future cases may help determine if D. vaginalis is likely to have an ongoing role in human pathology moving forward.
Interestingly, just prior to developing his mycotic aneurysm this patient had returned from a trip to Japan, which included some rural areas, and while there he had suffered from a flu-like illness causing a cough and generalised joint aches. It seems plausible that these symptoms could represent the early stages of infection by D. vaginalis. Alternatively, an acute viral infection may have made the patient more susceptible to opportunistic infection by D. vaginalis.
Conclusion
This case represents the first reported instance of D. vaginalis as a potential causative agent in a mycotic abdominal aortic aneurysm. Isolation of this bacteria from clinical specimens should be reported to aid our understanding of its potential pathogenic role in opportunistic infections.

Article DOI:
Journal Reference:
J.Vasc.Soc.G.B.Irel. 2025;5(1):31-33
Publication date:
September 16, 2025
Author Affiliations:
1. Medical Sciences Division, University of Oxford, Oxford, UK
2. Department of Microbiology and Infectious diseases, Oxford University Hospitals, NHS Foundation Trust, Oxford, UK
3. Wolfson Centre for Prevention of Stroke and Dementia, Nuffield Department of Clinical Neurosciences, University of Oxford, UK
4. Department of Vascular Surgery, Oxford University Hospitals NHS Foundation Trust, UK
Corresponding author:
Dr Simon N Williams
St Catherine’s College,
University of Oxford, Oxford,
OX1 3UJ, UK
Email: [email protected]











