CLINICAL AUDIT
An audit of glycaemic control and impact on surgical outcomes among inpatients with critical limb-threatening ischaemia (CLTI)
Tippireddy R, Barki D, El-Tayer O, Ng J, Nair H, Sandford R
Plain English Summary
Why we undertook the work: Many people in hospital with severe lower limb circulation problems (CLTI) also have poorly controlled blood sugar. When blood sugar isn’t well managed, wounds are slower to heal. High blood sugar after surgery increases the risk of serious problems with the affected limb, including possible amputation.
What we did: We reviewed hospital patients with CLTI over a 6-week period to see how well their blood sugar was controlled and how this affected outcomes. The review took place at one specialist vascular centre and included all such patients admitted during that time. We compared their blood sugar control against national guidelines and used statistical analysis to see if it was linked to outcomes after treatment.
What we found: Out of the hospital patients with CLTI, a small proportion had well-controlled blood sugars, while most had poor control. Patients with good blood sugar control healed better, had fewer amputations, and experienced fewer serious complications. Poor blood sugar control was strongly linked to worse healing and higher risk of amputation, even after accounting for other health factors. All deaths occurred in patients with poor blood sugar control.
What this means: This audit shows that even in a specialist diabetic foot centre, many patients have poor blood sugar control, which continues to worsen outcomes. Practical strategies and care pathways are needed to improve blood sugar management across all settings for this high-risk group of patients.
Abstract
Background: Diabetes mellitus is a key risk factor for peripheral arterial disease (PAD), with poor glycaemic control in diabetic patients linked to foot ulceration, delayed wound healing and an increased need for surgery and amputations. Most UK vascular centres have specialist multidisciplinary diabetes foot clinics to address this. Despite these efforts, diabetic foot complications, often associated with PAD, remain prevalent. We conducted an audit of inpatients with critical limb-threatening ischaemia (CLTI) to assess their glycaemic control and correlate it with limb-related outcomes.
Methods: Data were collected from a single tertiary vascular centre with focus on inpatients with CLTI over a 6-week period from 2 January 2023 to 12 February 2023, including all admitted patients during this time frame. Glycaemic control was audited against national guidelines. A multivariate analysis examined the relationship between HbA1c/blood glucose levels and post-procedural outcomes, adjusting for age, body mass index (BMI) and sepsis status, with glycaemic control categorised according to National Institute of Health Care and Excellence (NICE) guidelines.
Results: Of 236 inpatients, 120 with CLTI had blood glucose or HbA1c data available. The cohort was mostly male (70.3%), with a median age of 70 years. Among them, 92 patients (76.6%) had type 2 diabetes, four patients (3.3%) had type 1 diabetes and 24 (20%) were not diabetic. Median HbA1c and glucose levels were 8.7% and 10.7 mmol/L, respectively. Based on NICE guidelines, 54 patients (45%) were well controlled (Group 1) and 66 patients (55%) were poorly controlled (Group 2). Foot outcomes were linked to diabetes control: primary healing was higher in Group 1 (42.5%) than in Group 2 (18.1%) (p=0.002). Group 1 had fewer minor amputations (11% vs 24%, p=0.002) and major adverse events (major amputation and death) (12.9% vs 33.3%, p=0.002). Multivariate analysis when adjusted for age, C-reactive protein and BMI along with the glycaemic status showed poor glycaemic control was significantly associated with poorer wound healing and amputations (p<0.01), but not with unplanned surgeries (p>0.05). Five deaths occurred, all in poorly controlled patients.
Conclusion: Many vascular inpatients with CLTI with or without diabetes have inadequate glycaemic control, which is associated with adverse outcomes. This audit highlights that, despite a well-established multidisciplinary diabetic foot service in a tertiary centre and known associations between poor glycaemic control and adverse outcomes, diabetes management remains suboptimal and continues to affect patient outcomes. There is a need for actionable pathways to improve glycaemic control across care settings for this high-risk population.
Introduction
Chronic limb-threatening ischaemia (CLTI) is the most severe presentation of peripheral arterial disease (PAD) and affects 1% of the population in the UK.1 PAD is a common disease among patients with diabetes mellitus,2 and the relative risk of PAD increases with increasing duration and severity of diabetes.3 As diabetes is a major driver of the disease severity by acting at the molecular and cellular level,4 many patients with CLTI are found to have poorly controlled diabetes with elevated blood glucose levels and HbA1c. Postoperative hyperglycaemia is associated with adverse events after lower extremity vascular procedures in patients with and without diabetes including infection, increased hospital utilisation (need for further procedures) and mortality.5 Studies have shown that, in patients with diabetes and CLTI, HbA1c levels of >6.8–8% are associated with major amputations.6,7 The cost of treating CLTI in patients with diabetes is higher than the health system treatment costs of either coronary artery disease or cerebrovascular disease,8,9 and these increased costs may be associated with higher rates of hospital admissions, procedures, medication costs and complications seen in this group.8,9 The National Institute for Health and Care Excellence (NICE) has issued guidelines for perioperative diabetes control, setting an HbA1c target of 48 mmol/mol (6.5%) in patients with both type 1 and 2 diabetes, and a blood glucose target of 9 mmol/L in type 1 and 8.5 mmol/L in type 2 diabetes. This is based on clear evidence of poorer outcomes after surgery for patients with poor diabetic control.5-7
The primary aim of this study is to evaluate the adequacy of glycaemic control in CLTI patients admitted to a tertiary vascular unit. In addition, we considered patient access to a specialist diabetes review when needed. Our secondary aim was to assess any potential correlation between glycaemic control and impact on postoperative outcomes.
Methods
Study design
This was a retrospective audit of inpatients in a single-centre tertiary level vascular unit. Patients presenting with CLTI, regardless of their diabetes status (as per global vascular guidelines 2019) over a 6-week period from 2 January 2023 to 12 February 2023, all admitted patients during this timeframe, were included in the study.
Data gathered included patient demographics, presenting complaint and the intervention proposed, blood glucose pre- and post-intervention, HbA1c values, sepsis status (C-reactive protein, CRP), body mass index (BMI), inpatient diabetes team review and post-procedural outcomes. The post-surgical outcomes in CLTI patients were categorised as primary wound healing, need for further unplanned operation, minor amputation, major amputation and death. Glycaemic control definitions were taken from the NICE guidelines as follows: diabetic patients: HbA1c <48 mmol/mol (6.5%) and blood glucose levels <8.5 mmol/L; non-diabetic patients: HbA1c <42 mmol/mol (6%) and blood glucose levels 7.8 mmol/L.
Statistical analysis
Data analysis was performed using descriptive statistics and multivariate analysis. Blood glucose levels and HbA1c levels are presented as mean and medians, and categorical/quantitative variables such as age, glycaemic control, CRP, BMI and post-procedural outcomes are presented as counts and/or absolute numbers and analysed with a multinominal logistic regression model using R software. P values <0.05 are considered as statistically significant.
Results
From 3 January 2023 to 12 February 2023, a total of 236 patients were admitted as inpatients to the vascular unit at St Thomas’ Hospital. One hundred and forty-five patients were identified with CLTI, the majority of which were diabetic (69%). Of these, 25 patients (17%) did not have blood glucose measurements available and therefore were excluded. Five (11%) non-diabetic patients had available HbA1c levels and 24 (53%) non-diabetic patients with blood glucose levels were included in the analysis. A final number of 120 patients were included in the study (see Figure 1).
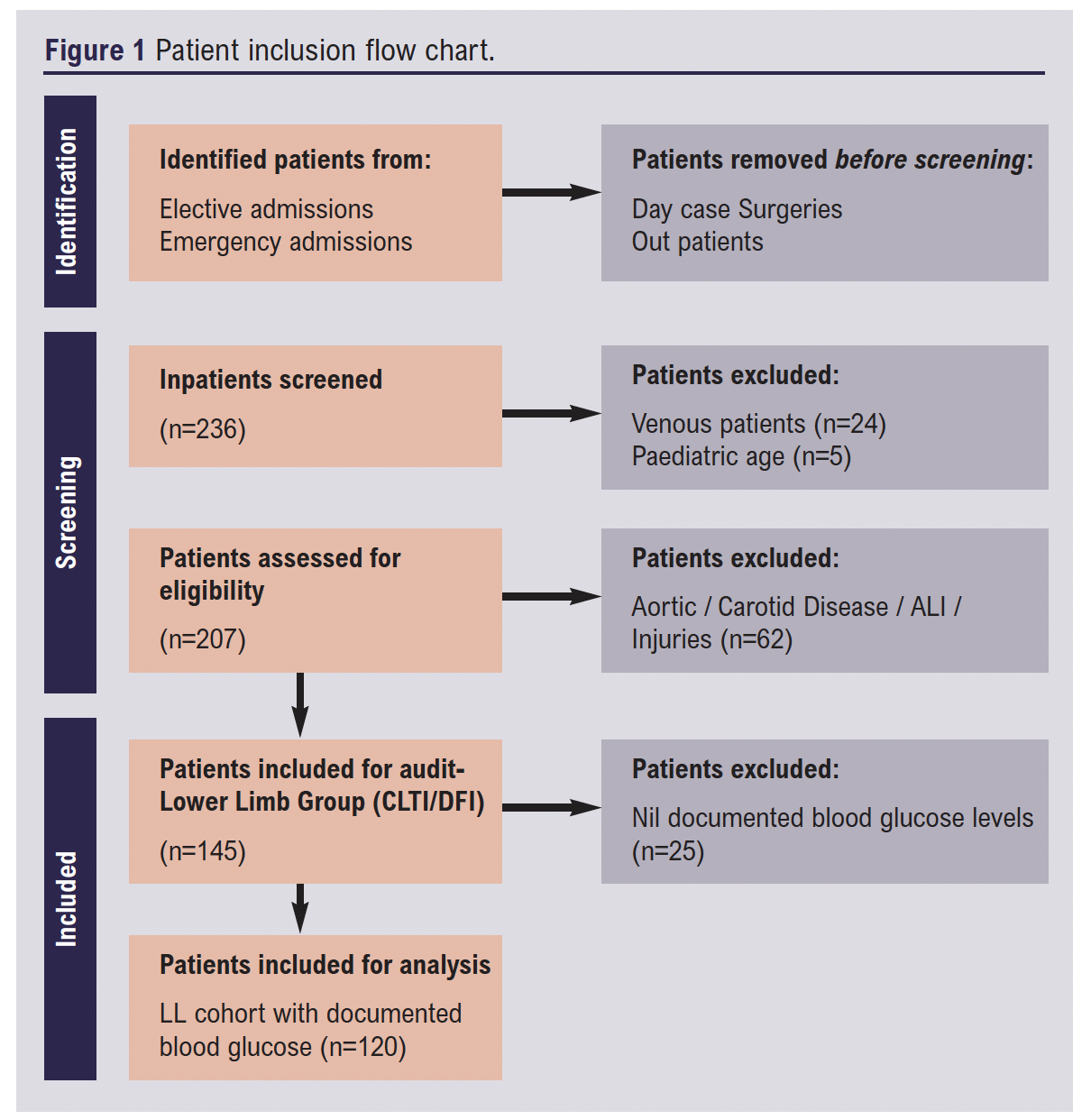
In the study group the median age was 70 years (range 38–92) and 85 (70.3%) patients were male. Ninety-six patients (80%) were known to be diabetic, of which four had type 1 diabetes and 92 patients had type 2. Twenty-four patients (20%) were not diabetic but had blood glucose and/or HbA1c levels available.
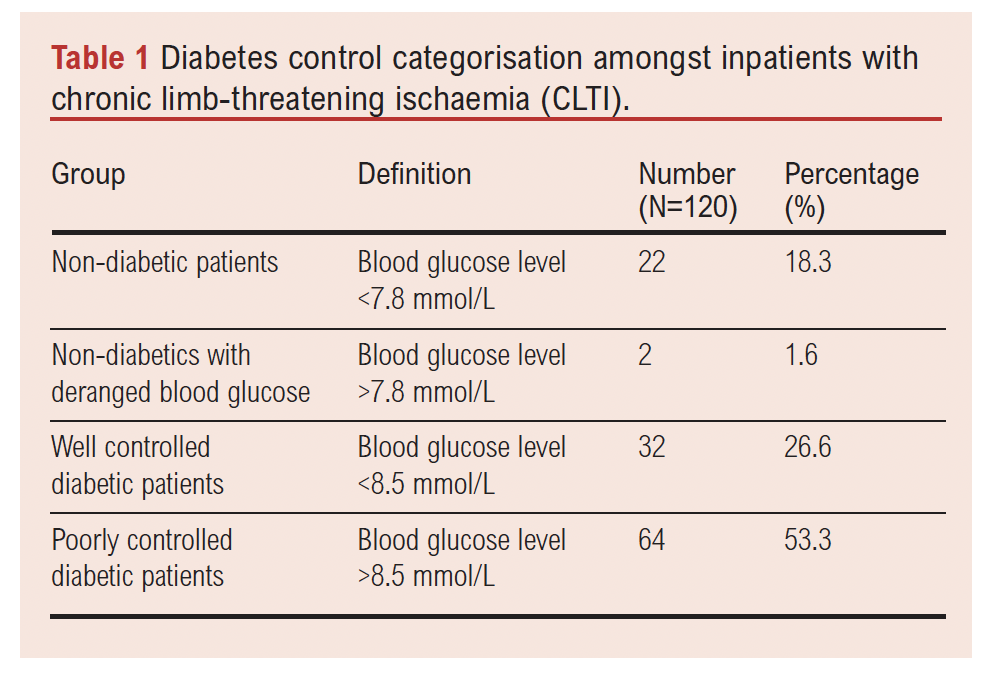
Fifty-four patients (45%) had well controlled blood glucose (<8.5 mmol/L) (Group 1), of which 32 (59%) were known to have diabetes and 22 (41%) were not diabetic. The median blood glucose level in this group was 6.5 mmol/L (range 4–8 mmol/L). Sixty-six patients (55%) had poorly controlled blood glucose (>8.5 mmol/L) (Group 2), of which 64 (97%) were known to be diabetic and two (3%) were not known to be diabetic. The median blood glucose level in this group was 12.8 mmol/L (range 2.1–27.4 mmol/L) (see Table 1).
Eighty-seven patients had documented HbA1c readings. Of these, 24 (27.5%) patients had well controlled HbA1c (<6.5%, 48 mmol/mol) including 20 diabetic patients and four patients without diabetes. The median HbA1c was 5.7%, 39 mmol/mol (range 5–6.4%). Sixty-three patients (72.4%) had poorly controlled HbA1c levels (>6.5%, 48 mmol/mol) including 62 diabetic patients and one patient without diabetes. The median HbA1c level for this group was 8.6%, 69 mmol/mol (range 6.2–16%).
There were 45 patients with CLTI who were not known to be diabetic. Of these, 24 patients had data available, of which two (8.3%) had poorly controlled blood glucose levels (>7.8 mmol/L) and one had an elevated HbA1c level of 46 mmol/mol (6.2%).
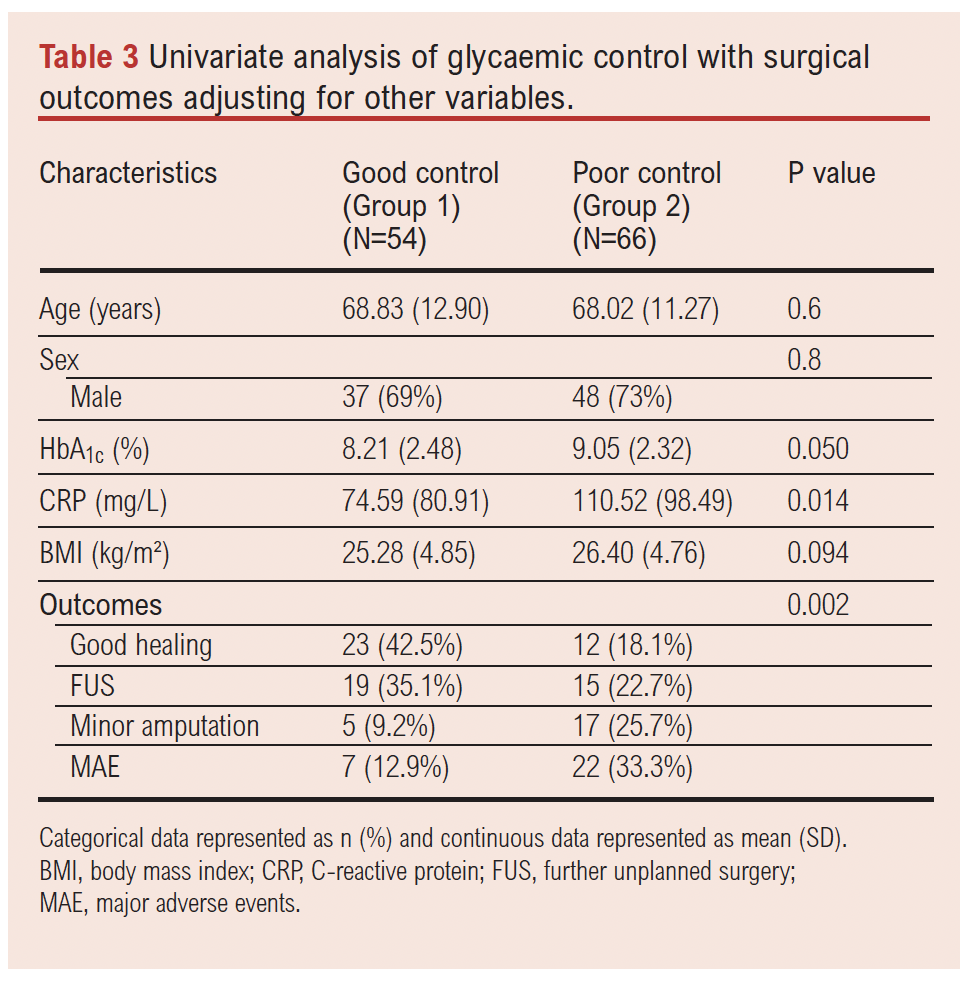
The median HbA1c in the group known to have diabetes for whom data were available (n=87) was 56.8 mmol/mol (7.7%), which was higher than the NICE recommendation of 48 mmol/mol (6.5%). The mean HbA1c for the good control group was 66 mmol/mol (8.2%) and for the poor control group was 75 mmol/mol (9.0%) (p=0.05). Further analysis of the relationship between sepsis (CRP) and glycaemic control was conducted and showed that the mean CRP level in the poor glycaemic control group was higher than in the good glycaemic control group (110.52 mg/L vs 74.59 mg/L; p=0.01).
Among the group with poorly controlled sugar levels (66 patients), 18 patients (27.2%) were reviewed as inpatients by the diabetes team. Two patients (3.7%) with well controlled sugar levels were reviewed by the diabetes team as inpatients.
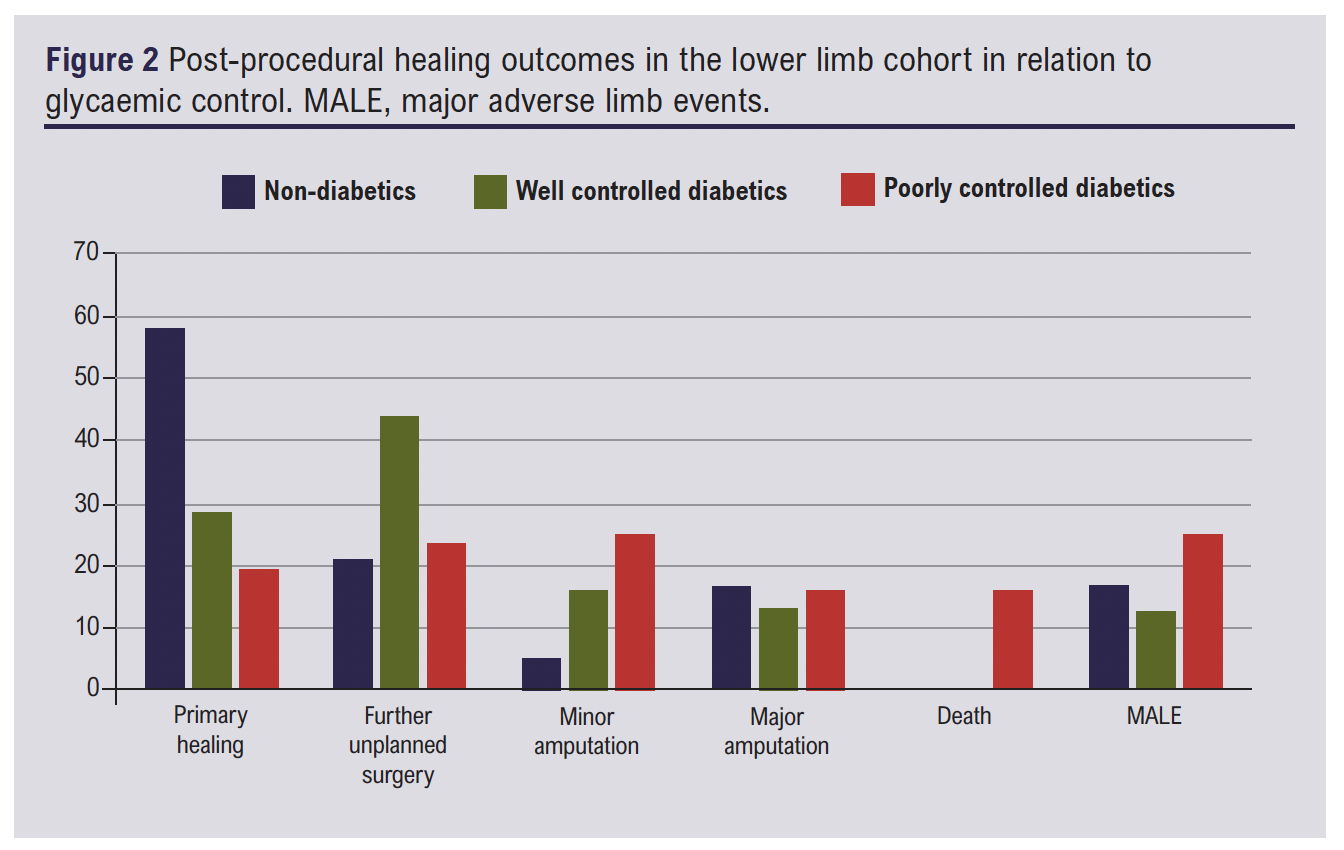
Univariate analysis showed that outcomes were correlated significantly with glycaemic control, with primary wound healing achieved in 42.5% (23/54) of patients with good glycaemic control and only 18.1% (12/66) of patients with poor glycaemic control (p=0.002). Further unplanned surgery was required in 35.1% (19/54) of patients with good glycaemic control and in 22.7% (15/66) of patients with poor glycaemic control (p=0.002). Minor amputations were more frequently observed in patients with poor glycaemic control (17/66 patients, 25.7%) compared with those who had well controlled sugars (5/54 patients, 9.2%; p=0.002; Table 2).
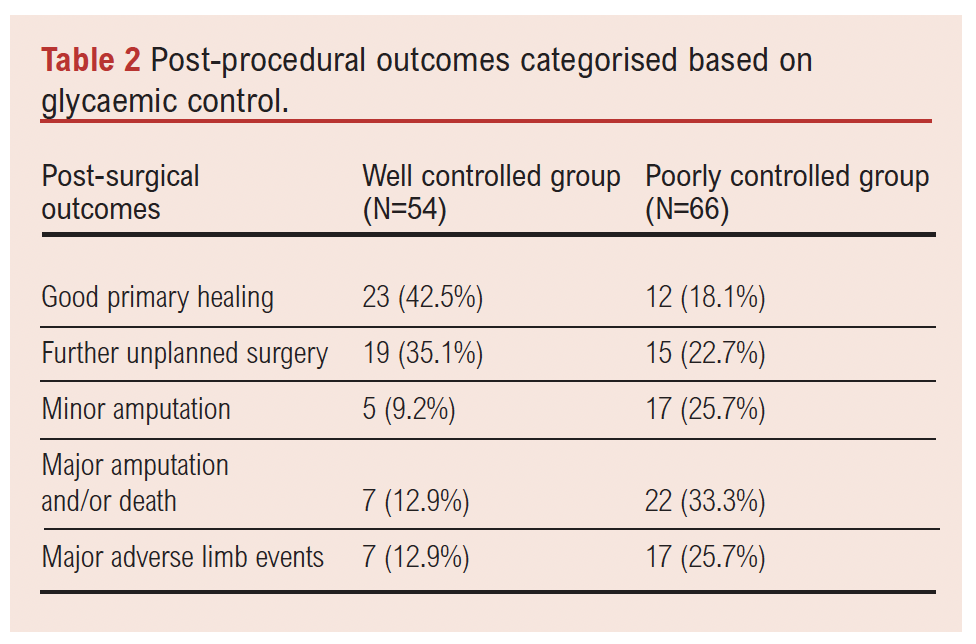
Major adverse limb events, defined as major limb amputation or further revascularisation of the index limb, were more common in the group with poor glycaemic control (17/66, 25.7%) than in the well controlled group (7/54, 12.9%; p=0.002) (see Table 3).
There were five (7.8%) deaths in this cohort, all of whom had poorly controlled diabetes (see Figure 2).
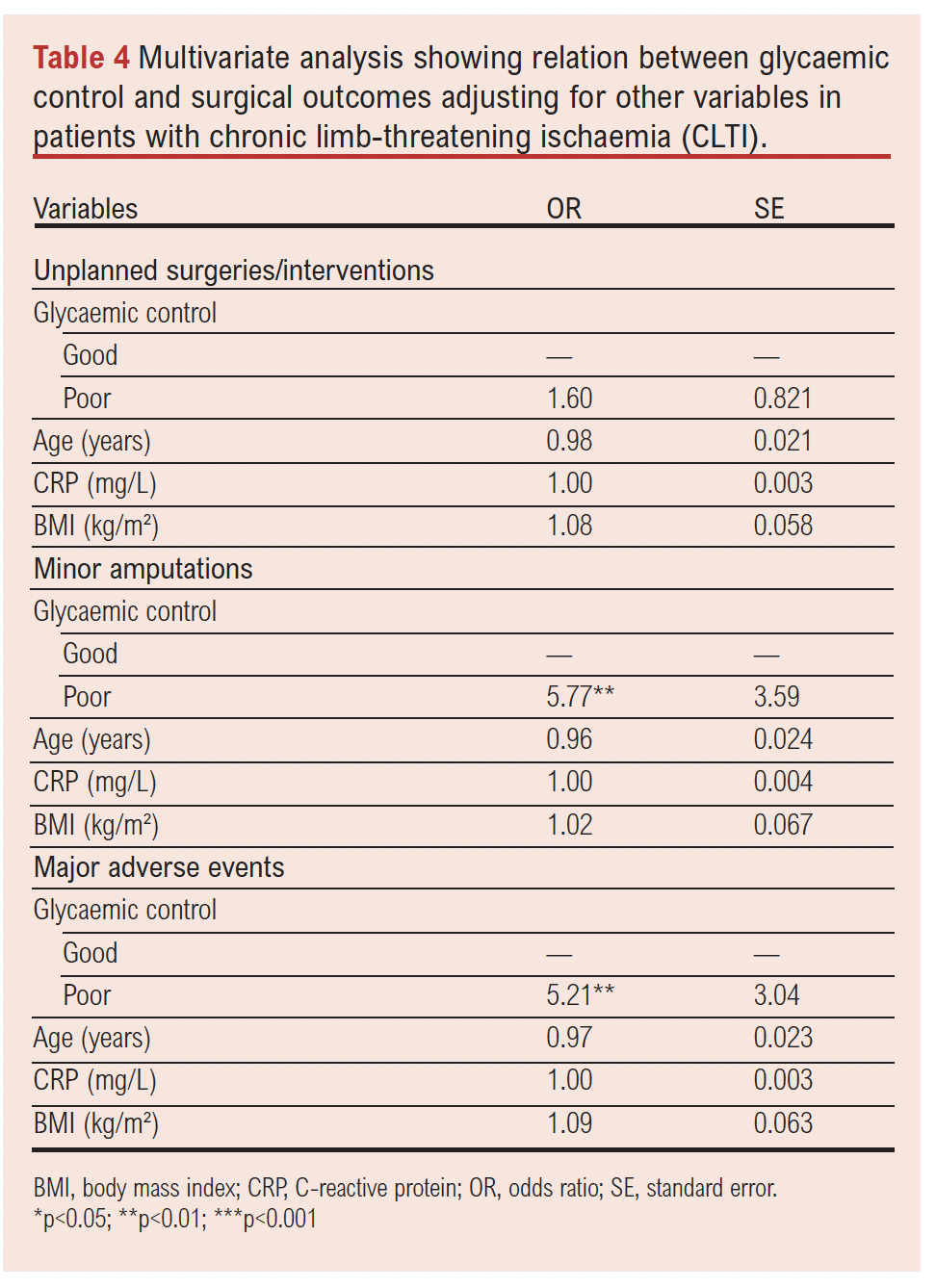
A multinomial logistic regression model analysed the relationship between glycaemic control and clinical outcomes, adjusting for age, CRP and BMI. In this regression model, poor glycaemic control was significantly associated with an increased risk of requiring minor amputations (p<0.01) and developing major adverse events (major amputation and/or death) (p<0.01), but was not significantly associated with further unplanned surgeries (p>0.05). Age, BMI and CRP levels did not seem to affect the results and are not the primary drivers of the clinical post-surgical outcomes (Table 4).
When the poorly controlled group (diabetic and non-diabetic) were compared with the combined well controlled group (diabetic and non-diabetic) there was a significant association with poorer rates of primary wound healing (18.1% vs 42.5%, p<0.01) and higher rates of minor amputation (25.7% vs 9.2%, p<0.01) and major adverse events (ie, major limb amputation and/or death) (33.3% vs 12.9%, p<0.01), whereas there was no statistically significant association with further unplanned surgeries when a multinominal analysis was performed (22.7% vs 35.1%, p>0.05; Tables 3 and 4).
Discussion
This contemporary audit of diabetes control among inpatients with CLTI was conducted primarily to assess compliance with NICE recommended glycaemic control targets in our cohort. It demonstrated a significant proportion of vascular inpatients with poorly controlled diabetes and correlated poorer outcomes in this group. Those with inadequate preoperative glycaemic control were three times less likely to achieve primary wound healing than those with well controlled or no diabetes. Major adverse limb events occurred in 25.7% of patients with poorly controlled diabetes compared with 12.9% of those with well controlled diabetes.
This finding is in keeping with published data demonstrating poorer surgical outcomes associated with inadequate glycaemic control.10
Yap et al11 observed that patients with CLTI with poor perioperative glycaemic control undergoing infra-popliteal revascularisation were at increased risk of restenosis, which could be a potential mechanism for the observation of lower primary wound healing rates and a greater need for further unplanned surgery in this patient group. In addition, deranged blood glucose levels can have a deleterious effect on the immune response at the wound bed and directly impact wound healing.12
Arya et al13 also found that poor perioperative glycaemic control, defined as HbA1c >7.0%, was associated with an increased risk of major adverse limb events such as amputation, in keeping with the findings of the present study. Another study including more than 2000 patients identified a greater risk of readmission within 30 days following an open or endovascular revascularisation in those with preoperative HbA1c of >6.5%.14 A further recent publication in 2024 partially agreed with the above, concluding that increased HbA1c is associated with a greater risk of early amputation.15 However, this study found similar outcomes following revascularisation for CLTI among patients with uncontrolled diabetes and those with well controlled diabetes.
In contrast to these studies and our currently presented data, Vogel et al5 did not find a significant difference in rates of major amputation associated with postoperative hyperglycaemia. However, this study confirmed the association between postoperative hyperglycaemia and other adverse outcomes including 30-day readmission, mortality and infectious complications. There was no difference in outcomes between patients with or without diabetes as hyperglycaemia was the main determinant factor.
This finding is corroborated by Kinio et al, who described hyperglycaemia as a factor in major adverse events following surgery including mortality, cardiac events and adverse limb events, regardless of diabetic status.10
A recent review noted that studies correlating outcome data with diabetes management often showed inconsistencies in variation of diabetes control definitions. This study has taken definitions of diabetes control from published national guidelines to overcome this potential weakness.16
There are some limitations to our study, which is a single-centre retrospective audit of current practice. As such, some data were missing from the electronic patient records and there may be unrecognised bias in the patients studied. However, it is a large busy tertiary vascular unit study, reflective of ‘real-world’ practice, and highlights a significant challenge in a highly complex patient group. Those with CLTI associated with diabetes are often found to have poor glycaemic control and, indeed, this may in part be a causative factor in their presentation. The urgent nature of revascularisation for CLTI to improve limb outcomes as recommended by national and international societies leaves little time for perioperative optimisation of diabetes control and other co-morbidities. Inpatient services across all specialties are struggling to meet current demands and therefore access to specialist diabetes team input within a short time frame can be difficult to achieve. Close collaboration between medical and surgical teams has led to the production of protocols to enable clinicians to address diabetic control in acute care settings (ie, THINK GLUCOSE guidelines).17,18 However, in these challenging cases there is likely to be benefit to more intensive and personalised support.
Conclusion
The current study goes some way to highlighting the challenges and impact of diabetes care on inpatient vascular patients with urgent lower limb presentations. Despite a dedicated multidisciplinary foot service within a tertiary vascular referral centre, glycaemic control in this high-risk cohort remains suboptimal, with an ongoing impact on patient outcomes. While recognising that the inpatient population may reflect a self-selecting higher risk group, current investment in multidisciplinary working has yet to achieve the desired improvements. These findings underscore the need to expand diabetes support beyond hub-site services, with greater emphasis on integrated community-based care – aligning with the direction of the NHS 10-year plan.
Further work is needed to understand what practically implementable solutions may improve glycaemic control and patient outcomes within the resources available. Identifying those at risk through ensuring blood glucose and HbA1c testing are conducted on admission is a vital first step which should be achievable in all cases, as evidence suggests that perioperative hyperglycaemia in non-diabetic vascular patients may adversely affect surgical outcomes to a similar extent as in diabetic patients. It will also be interesting to explore the preoperative journey of these patients, highlighting community and primary care-based opportunities to act where possible through, for example, strengthened multidisciplinary foot clinics in community settings. Local responses to these challenging patients will depend on local resources and protocols. However, highlighting those at risk to specialist diabetes teams should form an integral component to care and be recognised as an important factor influencing outcome.

Article DOI:
Journal Reference:
J.Vasc.Soc.G.B.Irel. 2025;4(4):223-228
Publication date:
August 27, 2025
Author Affiliations:
Academic Department of
Vascular Surgery, St Thomas’ Hospital, Guy’s and St Thomas’ NHS Foundation Trust,
London, UK
Corresponding author:
Ravali Tippireddy
Academic Department of Vascular Surgery, Floor 1,
North Wing, St Thomas’ Hospital, Guy’s and St Thomas’ NHS
Foundation Trust, Westminster Bridge Road, London
SE1 7EH, UK
Email: [email protected]











