ORIGINAL RESEARCH
Effect of health literacy and socioeconomic deprivation on outcomes after lower limb surgical revascularisation for chronic limb-threatening ischaemia: the HeaLTHI study
Bishop C,1 El-Sayed T,1 Baljer B,1 Buckley E,1 Convill J,1 Rowlands G,2 Bell R,1 Nandhra S,1,2
Plain English Summary
Why we undertook the work: Health literacy refers to the ability of patients to understand information related to their health condition so that they can make informed decisions about their health. Moreover, it is also believed that patients from disadvantaged backgrounds who have poor health are more likely to suffer from negative health outcomes. Therefore, we wanted to know whether this is true among our patients with poor leg circulation, particularly in its severe form which is called chronic limb-threatening ischaemia (CLTI) when they are undergoing surgery to improve their leg circulation.
What we did: We looked at patients who underwent major surgery for this disease (CLTI) in the Northern Vascular centre, Freeman Hospital, Newcastle upon Tyne, UK, and we asked them questions to see how much they understand about their condition, and we worked out how much advantaged or disadvantaged background they came from to know if that had any effect on how they did after surgery.
What we found: Our study found that a significant portion of patients with CLTI lacked knowledge about their condition and lived in poor areas. Unfortunately, we discovered that patients who lacked knowledge about their condition and hailed from poor areas were more likely to have complications after surgery.
What this means: Our research found that a patient’s understanding of their health condition and the financial and social environment they live in can impact their recovery after surgery to improve their poor leg circulation. However, more studies are needed to better understand this relationship with a larger sample of patients.
Abstract
Introduction: Research has suggested a relationship between health literacy, socioeconomic status and health-related outcomes. The aim of the study was to study the association between health literacy, socioeconomic status and outcomes following infra-inguinal bypass surgery for chronic limb-threatening ischaemia (CLTI).
Methods: Patients with CLTI undergoing lower limb surgical bypass graft operations between January 2016 and December 2018 were included in a cross-sectional observational study. The HLS19-Q12 questionnaire categorised participant’s health literacy as inadequate, problematic, sufficient or excellent. Socioeconomic status was assessed using the Index of Multiple Deprivation (IMD). Primary outcomes were major lower limb amputation (MLLA) and adverse cardiovascular events. Secondary outcomes included length of hospital stay, and early postoperative complications including pneumonia, surgical site and graft infection. Kaplan–Meier survival curves were used to compare health literacy and amputation, and Cox proportional regression analysis was conducted to identify differences in limb loss risk against health literacy and social deprivation levels.
Results: The study consisted of 50 patients with an average age of 70±8.7 years. The participants’ levels of health literacy were classified as inadequate (28%), problematic (38%), sufficient (24%) or excellent (10%). Approximately 40% of the patients lived in the most deprived areas. While all health literacy groups had similar postoperative outcomes, low health literacy was connected with lower socioeconomic status (r=0.308, p=0.029). IMD (p=0.017, HR 0.502 (95% CI 0.285 to 0.883)) and haemoglobin (p=0.001, HR 0.919 (95% CI 0.872 to 0.968)) were significant predictors of MLLA.
Conclusion: Patients with lower health literacy are more likely to face higher levels of social deprivation, which may predict amputation following bypass surgery. Enhancing health literacy could play a role in reducing health disparities caused by social deprivation, thereby potentially addressing a vascular James Lind Alliance priority.
Introduction
Health literacy is the degree to which individuals have the capacity to obtain, process and understand basic health information and access services needed to make appropriate health decisions.1 Health literacy is a complex concept that is influenced by an individual’s educational attainment, race, age, deprivation and available healthcare services.2,3 There are a number of health literacy assessment tools available, including the Rapid Estimate of Adult Literacy in Medicine (REALM) test, the Test of Functional Health Literacy in Adults (TOFHLA), the Newest Vital Sign (NVS) and the 12-item European Health Literacy Survey (HLS19-Q12), which is a brief self-administered questionnaire that was developed by the European Health Literacy Survey (HLS) Consortium and been validated as a reliable measure of health literacy.4
Social deprivation has been associated with low health literacy, and is defined as the lack of access to the resources and opportunities that are considered to be essential for individuals to participate fully in society.1,5 There are a number of social deprivation assessment tools available, including the Townsend deprivation index and the Carstairs deprivation score, which are based on census data, while the Index of Multiple Deprivation (IMD) is a composite measure of income, employment, education, housing and health.
Socioeconomic status is a social determinant of health and individuals with lower socioeconomic status have poorer health outcomes. Data support the association between social deprivation and health inequalities.6 Social deprivation and health inequalities are particularly pertinent in vascular patients because vascular disease is strongly related to lifestyle through behaviours such as smoking, poor diet and lack of physical activity.7,8 Chronic limb-threatening ischaemia (CLTI) is the severe presentation of peripheral arterial disease (PAD), producing ischaemic rest pain and tissue loss, reduced quality of life, and high risk of limb loss and/or mortality as well as increased cost and demand on vascular services.9 Low health literacy can compromise a patient’s adherence to lifestyle modification advice, medication compliance and the ability to seek medical advice when required.1,5 Unfortunately, these are essentials in the management of PAD including CLTI. Inadequate health literacy was doubled among socially deprived cardiovascular patients compared with high socioeconomic status patients. These patients had lower rates of access to health services, late presentation and poorer clinical outcomes.10-12 Previous reports suggested that socially deprived vascular patients are at an increased risk of amputation up to 65% compared with the least deprived populations in the UK and the USA.13-15
Social deprivation and poor health behaviours not only contribute to disease development, but also to clinical outcomes after vascular intervention.7,16-18 For example, peri-revascularisation smoking increases the risk of early major revascularisation bypass graft failure and limb loss.19,20 Therefore, social deprivation is associated with an increased risk of major amputation following revascularisation, in contrast to patients with income above the poverty line.21-23 A recent study suggested that over three-quarters of vascular patients had inadequate health literacy,24 with an increased risk of hospital readmission, cardiovascular disease and mortality.25-28 Therefore, understanding the relationship between health literacy and CLTI post-revascularisation outcomes is important given that health literacy is a potentially modifiable factor.1 Therefore, there is a need for a better understanding of health literacy in this vascular patient group.
This study aimed to assess the relationship between health literacy, social deprivation and clinical outcomes in CLTI patients who have undergone revascularisation surgery.
The study primary research question was: Is health literacy associated with postoperative clinical outcomes in patients with CLTI following lower limb revascularisation surgery? Secondary research questions were: (1) Is there an association between health literacy score and social deprivation score in CLTI patients? and (2) Is the social deprivation score associated with poor clinical outcomes in patients with CLTI following lower limb revascularisation surgery?
Methods
Study design and population
This is a single-centre cross-sectional prospective study of all patients aged >18 years who underwent infra-inguinal lower limb bypass graft surgery for CLTI between January 2016 and December 2018 in the Northern Vascular Centre, Freeman Hospital, Newcastle upon Tyne. CLTI was defined by at least two weeks of ischaemic rest pain, lower limb ulceration or gangrene.
Health Research Authority and Research Ethics Committee approvals were granted (21/NI/0092) with subsequent Newcastle upon Tyne Hospital research and development department approvals. Informed consent was obtained from all participants.
Procedural data
All patients with CLTI included in the study underwent infra-inguinal lower limb bypass surgery with either autologous vein or prosthetic graft. Patients who underwent endovascular interventions only were not included in the study as primary endovascular procedures are mainly done as day case procedures which makes recruiting and assessing their health literacy more challenging compared with open/hybrid interventions, considering the intervention technicalities have little influence or relevance to the study question. All patients had their regular clinical follow-up as well as research team follow-up with median follow-up of 12 months.
Baseline data collection
Baseline characteristics including demographics and comorbidities were collected by the research team from the patients’ electronic healthcare records. Laboratory tests collected include preoperative haemoglobin, sodium, creatinine and estimated glomerular filtration rate.
Comorbidities are defined as per the Society of Vascular Surgery (SVS) guidelines where possible.29 Diabetes is defined by documented medical history, the use of oral antidiabetic agents or insulin or fasting plasma glucose levels of at least 1.26 g/L; hypertension is defined by documented medical history and use of antihypertensive drugs for this purpose, or systolic blood pressure of at least 140 mmHg or diastolic blood pressure of at least 90 mmHg at admission determined by the average of the first two measurements. The following diseases were recorded based on the patient’s documented medical history: ischaemic heart disease or prior myocardial infarction, atrial fibrillation, hypertension, cerebrovascular disease (stroke, including ischaemic or haemorrhagic stroke as well as transient ischaemic attack), end-stage renal failure, renal failure defined as estimated glomerular filtration rate of <15 mL/min/1.73 m2 and/or requiring dialysis, and/or its documentation in their health records and a documented diagnosis of chronic obstructive pulmonary disease.
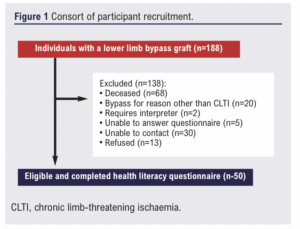
Inclusion criteria (Figure 1)
• Patients aged >18 years.
• Patients who have undergone lower limb revascularisation surgery for CLTI at Newcastle upon Tyne Hospitals NHS Foundation Trust between 1 January 2015 and 1 January 2019.
• Patients able to consent to study participation.
• Patients able to answer the health literacy questionnaire.
• Patients who can speak/understand English.
Exclusion criteria (Figure 1)
• Patients aged <18 years.
• Patients who have had lower limb revascularisation surgery for any reason other than CLTI.
• Patients who have had endovascular intervention even for CLTI.
• Patients who have had redo lower limb intervention even for CLTI.
• Patients who are unwilling to consent to study participation.
• Patients with incomplete data sets on the Northern Vascular Centre Register.
• Patients who are unable to speak/understand English.
Socioeconomic status
Socioeconomic status was determined using the Office for National Statistics English Indices of Multiple Deprivation (IMD) 2019 measure.30 This is a measure of relative deprivation and is calculated for each Lower-layer Super Output Area in England. The IMD tool graded participants’ postcode areas, ranking them from 1 (most deprived) to 10 (least deprived).
Health literacy
Health literacy was assessed using the 12-item European Health Literacy Survey (HLS19-Q12).4 Each response on the HLS19-Q12 was assigned a numerical value ranging from 1 to 4. Subsequently, a total score ranging from 1 to 50 was calculated for each patient, following the HLS19 scoring system. Based on these scores, patients’ health literacy was classified into four categories: inadequate (score 0–25 points), which is the severe level of poor health literacy; problematic (score >25–33 points), which is the moderate level of poor health literacy; sufficient (score >33–42 points), which is the mild level of poor health literacy; and excellent (score >42–50 points).
Postoperative outcomes encompassed major lower limb amputation (below, through or above the knee joint) and early postoperative complications including myocardial infarction, hospital acquired pneumonia, 3-month graft occlusion (first postoperative graft surveillance ultrasonography scan), surgical site infection (when documented in the patients’ hospital/healthcare records and defined as an infection that occurs at the site of the bypass and associated with cellulitis and/or purulent discharge) and raised inflammatory markers (leucocyte count and/or C reactive protein level).31 Graft infection was diagnosed when documented in the patients’ hospital/healthcare records and associated with overlying cellulitis, the presence of an exposed prosthetic graft, sinus tract with persistent purulent drainage and/or bleeding, or palpable anastomotic pseudoaneurysm. This is in addition to elevated inflammatory markers such as leucocyte count and/or C-reactive protein levels, and radiological evidence such as peri-graft fluid and/or gas, graft disruption and pseudoaneurysm formation observed on ultrasonography and computed tomography images.32
Study outcomes
The primary outcome was to identify the association between health literacy and postoperative outcomes following lower limb revascularisation surgery for CLTI. Secondary outcomes included: (1) to identify if socioeconomic status was associated with an increased risk of limb loss (amputation-free survival) or mortality following lower limb revascularisation surgery for CLTI; and (2) to understand the relationship between socioeconomic status and health literacy scores.
Statistical analyses
Normally distributed data were presented as mean (SD) and hypothesis testing was performed with paired and unpaired t-tests. Categorical data were analysed by means of a χ2 test. A generalised linear model/Kruskal–Wallis test was used for comparison of mean/median continuous data between groups. IMD quintiles and health literacy categories were treated as ordinal and analysed with rank correlation. Spearman’s rank correlation test was performed between IMD and health literacy. Kaplan–Meier survival curves were used with a log-rank test to compare health literacy and amputation. A Cox proportional regression analysis was conducted to identify differences in limb loss to enable hazard analysis. An a priori power analysis was conducted using G*Power3 to test the primary outcomes and survival analyses, with an alpha of 0.05.33 The results showed that a minimum sample of 48 and 35 participants were required, respectively, to achieve a power of 90%. A p value of <0.05 was considered statistically significant. Statistical analysis was performed using SPSS version 24 (IBM SPSS Statistics for Windows, Version 24.0. IBM Corp, Armonk, New York, USA).
Results
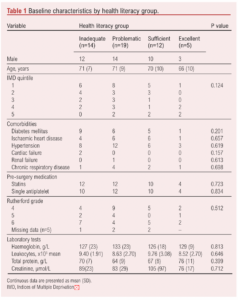
A total of 50 participants were included in the study (39 males, 78.0%) with a mean±SD age of 70±8.7 years and median follow-up of 12 months. Fourteen patients (28%) had inadequate health literacy, 19 (38%) had problematic health literacy, 12 (24%) had sufficient health literacy and 5 (10%) had excellent health literacy. Twenty-five participants (50%) lived in areas of highest deprivation (IMD 1–3), 11 participants (22%) lived in areas of moderate deprivation (IMD 4–6) and 14 (28%) lived in areas of lowest deprivation (IMD 7–10). Baseline demographics were comparable between health literacy groups (Table 1).
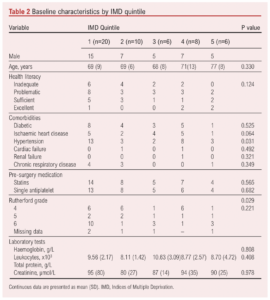
A significant difference was found between IMD groups based on the degree of severity of lower limb ischaemia as outlined by the Rutherford grade at the time of intervention (p=0.029) and hypertension (p=0.031) (Table 2). Health literacy was weakly but significantly correlated with IMD score (r=0.308, p=0.029).
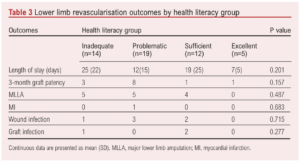
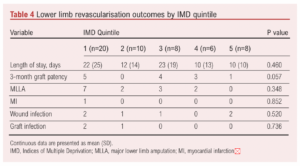
There were no significant differences in postoperative outcomes between health literacy groups (Table 3) or IMD quintiles (Table 4), including length of stay, 3-month graft patency, MLLA and myocardial infarction.
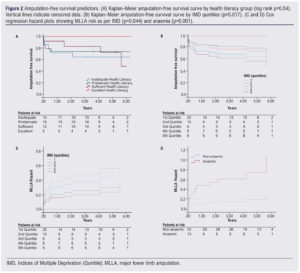
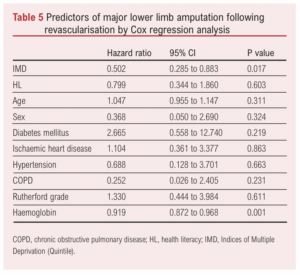
The mortality rate over the 12-month period according to health literacy and IMD groups was as follows: Health literacy: inadequate 21.42%, problematic 15.78%, sufficient 8.33%, excellent 0.00%. IMD: 1st quintile 30%, 2nd quintile 10%, 3rd quintile 33.3%, 4th quintile 12.5%, 5th quintile 0.00%. Kaplan–Meier analysis revealed no significant difference in amputation-free survival between health literacy groups (log rank p=0.545) and IMD groups (log rank p=0.887) (Figure 2A). Cox regression analysis showed that IMD (p=0.017, HR 0.502 (95% CI 0.285 to 0.883)) and haemoglobin (p=0.001, HR 0.919 (95% CI 0.872 to 0.968)) were significant predictors of MLLA (Table 5). Only one patient developed postoperative myocardial infarction, so Cox regression could not be calculated for this outcome.
Discussion
To our knowledge, this is the first study to investigate the association between health literacy among patients with CLTI undergoing lower limb revascularisation bypass surgery and postoperative outcomes. We found that socioeconomic status is associated with the health literacy level and the degree of severity of vascular disease in patients who underwent vascular intervention for CLTI. Social deprivation level measured by IMD was found to be a significant predictor of major adverse limb events; however, there was no significant difference in major adverse clinical outcomes among health literacy groups.
Our study cohort showed a weak correlation between health literacy and IMD. This correlation was also demonstrated by a previous report and showed that lower socioeconomic groups are more likely to have low health literacy, resulting in poor health status. This is because health literacy was shown to mediate the relationship between socioeconomic status and health status, quality of life and health-related outcomes. This could be particularly true in patients with PAD as their socioeconomic status is likely to influence their health behaviours such as smoking, poor diet and physical activity.34,35
Approximately half of our study population were from areas of high levels of social deprivation. Patients from high levels of social deprivation were likely to have inadequate health literacy, as a significant correlation was found between socioeconomic status and health literacy (p=0.029). This was better explained when 70% of participants in the lowest IMD quintile had inadequate or problematic health literacy, while in the highest IMD quintile only 33% had problematic health literacy. This is comparable to the European study which found limited health literacy in 73.9% of individuals with low social status.36
Although no difference was found in postoperative outcomes between IMD groups, similar to a UK multiple national databases study, there was no association between patients’ socioeconomic deprivation and one-year postoperative death following major amputation for CLTI, but the authors concluded that the relationship between social deprivation and CLTI is potentially more complex and suggested a prospective investigation of this relationship.37 However, our Cox regression analysis showed that IMD was a significant predictor of major lower limb amputation. This finding is supported by previous studies that showed patients from deprived areas were 2.4 times more at risk of amputation compared with less deprived areas.38
In our cohort, although not statistically significant, participants from areas of highest deprivation were younger (69 years) compared with the participants in the lowest deprivation areas (77 years). Previous reports have found individuals from high deprivation areas presented with similar pathology and comorbidities at a younger age compared with their less socially deprived counterparts.39
In our patient cohort, none of the participants with excellent health literacy had an amputation. One could assume that excellent health literacy could be a protective effect against major amputation. Nevertheless, caution is advised as the ‘excellent health literacy group’ was small in this study (n=5), and a larger cohort of patients in a wider study is needed for better evaluation of this association.
The majority of our participants (66%) had inadequate or problematic health literacy, which is considerably higher than the 47.6% of individuals with inadequate or problematic health literacy in a previous European study.31 Similar high rates of low health literacy (76.7%) were reported among PAD clinic patients in the Netherlands.21 Limited data exist for a comparison of health literacy in England. Although our cohort of patients did not show a significant difference in postoperative outcomes among health literacy groups, other surgical areas have found significant differences. For example, patients with poor health literacy spent a longer time in the hospital following major abdominal surgery and suffered from an increased risk of complications such as surgical site infections and, when they were discharged, they had decreased compliance with discharge instructions including medication compliance and wound/drain care.40-42
Social deprivation combined with reduced health literacy can be linked with an increased display of poor lifestyle behaviours including smoking, poor diet and inadequate physical activity leading to poorer health outcomes. This could be particularly true in patients with PAD as their socioeconomic status is likely to influence their health behaviours such as smoking, poor diet and physical activity, which are common risk factors for PAD and amputation.8,43-45
Lack of awareness of vascular disease symptoms and inequalities in access to healthcare services may lead to socially deprived patients presenting with more advanced vascular disease at a younger age. Requiring surgical intervention at a younger age could result in higher disability life-years experienced and more life-years lost, therefore leading to reduced health-related quality of life.39,46
Recent studies have shown that patients with adequate health literacy will have the knowledge, skills and confidence to navigate the healthcare system, leading to more efficient use of healthcare services and better health outcomes.35,47 Improving health literacy could therefore have a mediating role in the relationship between social deprivation and health outcomes through health literacy interventions. This could improve the outcomes for patients with PAD following vascular intervention.
In this study we have shown that health literacy could be a social determinant of health, as health literacy follows a social gradient and creates health inequalities. We believe health literacy is a potentially modifiable factor and could be a facilitator in reducing the gap in health inequalities and social deprivation, with subsequent improved health outcomes.35,47 Health literacy intervention remains in its infancy, with most research being conducted in the USA, including patient-centred communication and self-management programmes.48,49
Health literacy is influenced by race and ethnicity as individuals from different cultures may struggle to navigate through the healthcare system due, for example, to language barrier, different levels of education and different beliefs about health and illness. A number of studies have shown that people from racial and ethnic minority groups are more likely to have low health literacy than those from white majority groups. For example, a study by the National Centre for Education Statistics found that 44% of African Americans and 42% of Hispanics had low health literacy compared with 28% of white subjects.50
Improving health literacy is recognised as a national imperative, prompting collaborative efforts between Health Education England, Public Health England and NHS England, and it was one of the foremost priorities identified by the James Lind Alliance for PAD management coupled with improving the educational support for patients with poor leg circulation. Therefore, health literacy enhancement could be a potential avenue for mitigating health inequities stemming from socioeconomic disadvantages, thereby aligning with a key vascular priority established by the James Lind Alliance.51 Health literacy interventions should be tailored at an individual level for an improved patients’ understanding and more efficient use of healthcare services, better health outcomes and improved quality of life for patients.2,3 As social deprivation and health literacy are linked, there may be merit in identifying vascular patients with a low IMD postcode and targeting these patients for perioperative risk modification to improve postoperative outcomes.39
Study limitations
The study has several limitations that should be acknowledged. First, the sample size was relatively small, consisting of patients from a single centre. Additionally, the study population was relatively homogenous, comprising individuals residing in the North-East of England. Therefore, the findings may not be generalisable to broader populations. Despite these limitations, the study provides valuable insights and warrants future investigation through larger multicentre prospective observational studies. These studies should aim to evaluate the impact of health literacy and social deprivation on patients with CLTI and their revascularisation outcomes.
Conclusion
This study provides valuable insights into the clinical implications of health literacy and social deprivation in patients with PAD. There is an association between poor health literacy and social deprivation among patients with CLTI. Patients with poor health literacy coming from socially deprived areas are at higher risk of MLLA following lower limb revascularisation for CLTI. Based on the findings of this study, tailored health literacy interventions could be implemented to mitigate the negative impact of low health literacy and social deprivation on postoperative outcomes.

Article DOI:
Journal Reference:
J.Vasc.Soc.G.B.Irel. 2023; 3(1): 10-18
Publication date:
November 8, 2023
Author Affiliations:
1. The Northern Vascular Centre, Freeman Hospital, Newcastle upon Tyne, UK
2. Population Health Sciences Institute, Faculty of Medical Sciences, Newcastle University, Newcastle upon Tyne, UK
Corresponding author:
Tamer El-Sayed
NIHR Clinical Lecturer in Vascular Surgery, The Northern Vascular Centre, Freeman Hospital, Freeman Road, High Heaton, Newcastle upon Tyne
NE7 7DN, UK
Email: [email protected]











